Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
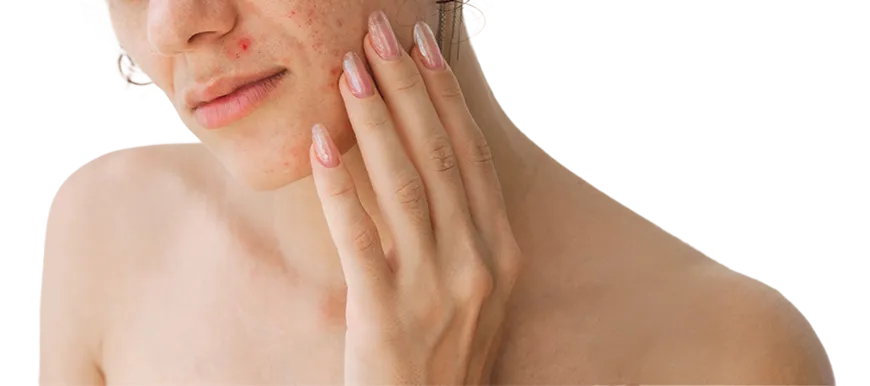
Acne scars develop when inflammation from acne damages the deeper layers of the skin, leaving behind indentations, raised scars, or uneven skin texture. While these scars usually do not fade completely on their own, modern dermatological treatments can significantly improve their appearance and overall skin smoothness.
At TSN Dermatology, treatment plans are tailored to the specific type and severity of acne scars. Using a combination of evidence-based techniques that stimulate collagen remodeling and improve skin texture, our goal is to achieve gradual, natural-looking improvement in the skin's surface and tone.




What Are Acne Scars?
Acne scars form when inflammation from acne damages the deeper layers of the skin. During the healing process, the skin may produce too little or too much collagen, which can result in either depressed (indented) scars or raised scars.
Acne scars are different from temporary post-acne marks. They represent permanent changes in the skin's structure, which is why they usually require specialised dermatological treatments to improve skin texture and smoothness.
What Are Common Types of Acne Scars?
Acne scars can appear in several forms depending on how the skin heals after acne. Some scars cause depressions in the skin, while others appear raised or thickened. Identifying the type of scar helps guide the most effective treatment approach.
Atrophic (Depressed) Scars
Atrophic scars are the most common type of acne scar. They occur when the skin does not produce enough collagen during healing, leaving visible depressions in the skin.
-
Ice-Pick Scars
Narrow, deep indentations that look like the skin has been punctured by a sharp object. -
Boxcar Scars
Broad depressions with well-defined edges. They may be shallow or deep and commonly appear on the cheeks and temples. -
Rolling Scars
These create a wave-like or uneven texture on the skin. They are caused by fibrous bands beneath the skin that pull the surface downward.
Pigmented or Discolouration Marks
Some acne lesions leave changes in skin colour rather than changes in texture. These marks may appear red, brown, or pale depending on how the skin heals.
-
Red Marks (Post-Inflammatory Erythema)
Persistent redness caused by dilated blood vessels near the skin surface. -
Brown Marks (Post-Inflammatory Hyperpigmentation)
Darker spots that occur when inflammation triggers excess melanin production. -
Pale or White Marks (Hypopigmentation)
Lighter patches that occur when the skin loses pigment or becomes thinner in the affected area.
Hypertrophic and Keloid Scars
These scars appear raised rather than depressed and develop when the skin produces too much collagen during healing.
-
Hypertrophic Scars
Thickened scars that remain within the boundaries of the original acne lesion and may gradually improve over time. -
Keloid Scars
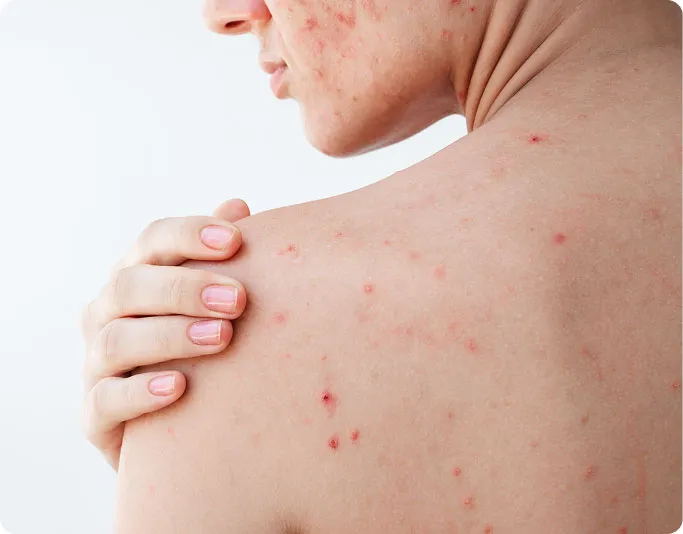
Raised scars that extend beyond the original acne site and may continue to grow. They are more commonly seen on the jawline, chest, shoulders, and back.
Common Symptoms of Acne Scars to Look Out For
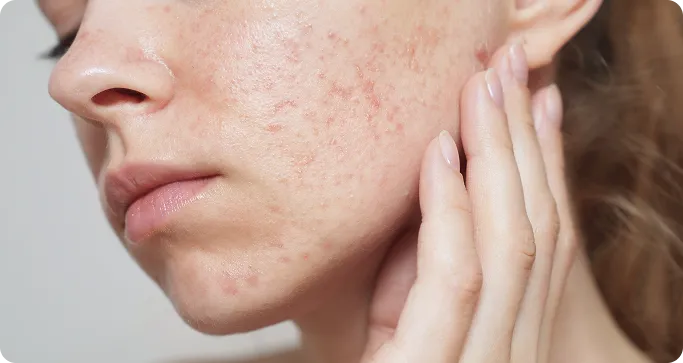
Acne scars can present differently from person to person, and their appearance often depends on the depth of the initial inflammation and your skin's unique healing response. While the severity varies, the following are the most common signs and features patients may experience.
Textural Depressions and Pitting
The most frequent symptom of atrophic scarring is a visible loss of skin volume. This manifests as:
-
Deep Puncture Marks
Narrow, deep pits that look like enlarged pores or ice-pick indentations. -
Defined Depressions
Shallow to deep box-like pits with sharp vertical edges or saucer-like dips that create an uneven skin surface. -
Undulating or Wavy Texture
A rolling appearance that is often most visible under side-lighting, caused by internal fibers pulling the skin down.
Raised or Thickened Skin
In some cases, the skin over-produces collagen during the healing process, leading to structural changes that sit above the surface:
-
Firm, Raised Bumps
Smooth, raised areas of skin that persist long after the acne has cleared. -
Thickened Scar Tissue (Keloids)
Rubbery, firm lesions that may grow larger than the original acne spot, commonly found on the jawline, chest, and back.
Persistent Redness and Discolouration
Scars are frequently accompanied by long-standing changes in skin tone that do not fade with standard over-the-counter products:
-
Red or Pink Marks (PIE)
Persistent red spots caused by dilated or damaged capillaries in the area of previous inflammation. -
Brown or Dark Spots (PIH)
Areas where the skin has produced excess melanin, resulting in tan or dark brown patches. -
Pale or White Patches
Areas where the skin has lost its natural pigment or become significantly thinned over time.
Tethering and Loss of Flexibility
Deep scarring can affect the structural integrity of the skin layers:
-
Fixed Depressions
Certain scars may appear anchored to the underlying tissue and do not disappear when the skin is stretched. -
Skin Rigidity
Long-standing cases of scarring can cause the skin to feel stiffer or less flexible in localized areas compared to surrounding healthy skin.
Social and Emotional Impact
While not a physical marking, the persistent nature of acne scars can significantly affect self-esteem and quality of life. Many patients report feeling the need to use heavy makeup to fill in the texture or avoid certain lighting environments due to the visible shadows cast by the scars.
What Causes Acne Scarring?
Not every acne breakout leaves a scar. Acne scars usually form when deeper inflammation damages the skin and affects the way it heals. Factors such as the severity of acne, repeated breakouts, and how the skin responds to inflammation can all influence whether a scar develops. Understanding what causes acne scars and the factors that trigger them can help with early treatment and prevention.
Deep-Seated Inflammation
Physical Trauma: Picking and Squeezing
Loss of Collagen Support
Delayed Treatment and Persistence
Genetic Predisposition
Environmental Factors: UV Exposure
How Are Acne Scars Diagnosed?
Diagnosing acne scars involves a careful assessment of your skin to determine the type, depth, and extent of the scarring. This is important because different types of acne scars respond to different treatments. During your consultation, a dermatologist will examine your skin and evaluate several factors to identify the most suitable treatment approach.
Skin Examination
Identification of Scar Types
Assessment of Scar Severity
Skin Type and Healing Tendencies
Personalised Treatment Planning
How is Acne Scarring Treated at TSN Dermatology?
Effective management of acne scars depends on the type of scar and the depth of the tissue damage. Because most patients present with a variety of scar types, we utilize a combination of clinical methods and repeated treatments to achieve optimal results.
It is important to note that treatment for acne scars should take place only after active, inflammatory acne is brought under control to prevent new scars from forming.

Individualised Treatment Approach
As acne scarring varies greatly from person to person, treatment must be customised. Treatment plans are tailored based on:
Types of Scars Diagnosed
Identifying the mix of atrophic (ice-pick, boxcar, rolling) or hypertrophic (raised) scars.
Extent and Location
Assessing the area of skin involvement, such as the cheeks, temples, or jawline.
Skin Tone and Sensitivity
Selecting technologies safe for specific skin types to avoid post-inflammatory hyperpigmentation.
Downtime Preferences
Balancing the intensity of treatment with your lifestyle and recovery requirements.
Advanced Laser Modalities
We provide modern and effective medical lasers to remodel collagen and correct discolouration.
Fractional Carbon Dioxide (CO2) Laser
We use the DEKA SmartXide CO2 laser, a newer version of the original SmartXide with DOT therapy. It combines high-degree technical features with evolved RF-CO2 laser source technology. By creating minute columns of heat in the skin, it stimulates the healing mechanism to form new collagen. Noticeable improvement in atrophic scars, wrinkles, and laxity can be seen after 2 to 4 sessions at 1- to 2-monthly intervals. Numbing cream is applied to minimize discomfort. After treatment, expect redness for 3 to 5 days and small amounts of crusting for 1 to 2 weeks.
Nd:YAG Laser
The BiAxis Q-switched Nd:YAG laser is an advanced, professional multi-purpose laser made in Germany. It is effective in treating both superficial (epidermal) and deep (dermal) pigmentation problems, including dark acne scars. There is usually very little downtime, though sun protection is essential to enhance the efficacy of the treatment.
Procedural Interventions
For structural scars that require more than just surface resurfacing, we perform other specialised procedures.
Subcision of Scars
Performed under local anaesthesia, a specialized needle-blade is inserted beneath the skin to break up the fibrous tissue (tethers) pulling the skin downwards. This releases rolling scars and stimulates new collagen to plump the area.
TCA CROSS
This stands for trichloroacetic acid chemical reconstruction of skin scars. It is a quick office procedure where a tiny amount of highly concentrated acid is applied to ice-pick or boxcar scars. This controlled injury stimulates the skin to fill up the scar. Scabs form a few days after and fall off in 1 to 2 weeks.
Surgical Removal of Scars
Some scars are best treated by cutting the scarred area away and gently stitching the normal skin back together. The resultant surgical scar is often less obvious and aesthetically superior to the original acne scar.
Skin Resurfacing and Peels
Chemical Peels
Using pharmaceutical-grade chemicals to remove the top layers of old and damaged skin, this process reveals fresher skin and stimulates new collagen formation. We typically use superficial to medium-depth peels to smoothen atrophic and superficial scars while minimizing the risk of side effects.
What to Expect Before and After Acne Scar Treatment
Acne scar treatments involve both preparation and aftercare to ensure safe healing and the best possible results. Understanding what to expect before and after your procedure can help you prepare for treatment and support your skin's recovery.
Getting Your Skin Ready for Acne Scar Treatment
Before your treatment, your dermatologist may recommend several preparation steps to help protect your skin and ensure the procedure is performed safely and effectively.
-
Clean and Clear Skin
Please ensure the areas being treated are clean and free of any creams, lotions, perfumes, or cosmetics. These products can create a barrier that interferes with laser precision or the depth of chemical penetration. -
Pause Active Skincare
Avoid using retinoids, prescription acne topicals, or exfoliating acids (such as AHAs or BHAs) for 3-5 days prior to your session, unless specifically instructed otherwise. These can sensitize the skin and increase the risk of irritation or delayed healing. -
Sun Protection
Avoid deliberate or unprotected sun exposure in the weeks leading up to your treatment. Tanned skin can interfere with laser safety settings, and accidental sunburn increases the risk of post-inflammatory hyperpigmentation (brown spots). -
Medication Awareness
Please inform our team of all current medications, especially if you are taking blood thinners. -
What to Wear
Wear comfortable, loose-fitting clothing that allows easy access to the treatment areas. For laser sessions, we will provide you with protective eyewear to be worn throughout the procedure.
Supporting the Healing Process After Acne Scar Treatment
After your treatment, following the recommended aftercare instructions can help protect your skin, support healing, and ensure the best possible treatment results.
-
Gentle Cooling
After procedures like Fractional CO2 laser or TCA CROSS, it is normal to feel a heat sensation. Follow your doctor's instructions for steps to keep the area cool, hydrated, and protected. -
Managing Crusts & Scabs
After treatments like TCA CROSS or fractional lasers, you may notice small crusts or scabs. Do not pick or scrub these off. Let them shed naturally over 1-2 weeks as picking can lead to infection and new scarring. -
Aggressive Sun Protection
Your skin is vulnerable to UV rays during the healing phase. When heading out into Singapore's tropical sun, use a broad-spectrum, non-comedogenic sunscreen (SPF 50+) and consider wearing a hat or seeking shade. -
Gentle Skincare
For the first week, avoid scrubs, toners, and active anti-ageing products.



When Should You See a Dermatologist for Acne Scars?
You should consider seeking professional dermatological care if your acne has left behind textural changes, if you are experiencing persistent redness or dark spots that do not fade over time, or if your scarring is negatively impacting your self-confidence and quality of life. While acne scars are not life-threatening, they have been linked to loss of self-esteem, particularly in adolescents and young adults. Specialist care is particularly important in the following scenarios:
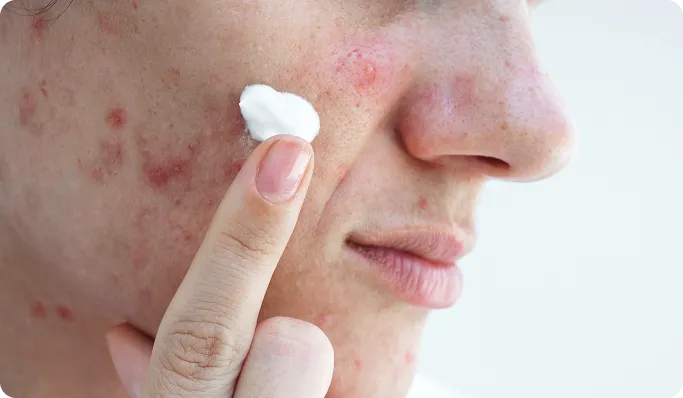
When Active Acne Persists
If you are still experiencing frequent, inflamed breakouts, you need a dermatologist to bring your acne under control first. Treating scars while active acne is ongoing is ineffective and can often lead to the formation of new, deeper scars.
When Over-the-Counter Products Fail
If you have tried various skincare routines without seeing an improvement in your skin's texture, it is likely that your scars are structural and require advanced interventions like laser therapy or subcision.
When Scars are Deep or Tethered
If you notice that certain scars look like deep pits or remain depressed when you stretch your skin, these are best treated by a medical professional.
If You Have a History of Keloids
If you or your immediate family members have a history of raised, thickened scars (keloids), specialised supervision is recommended to ensure that any treatment performed does not trigger excessive tissue growth.
FAQs About Acne Scar Treatment
Acne scars can be significantly improved with treatment, but they are not always completely removed. The degree of improvement depends on factors such as the type of scars, their severity, and your skin's healing response. In many cases, a combination of treatments performed over several sessions can achieve noticeable and long-lasting improvement.
Most acne scar treatments are generally well tolerated. Before the procedure, a topical numbing cream is usually applied to reduce discomfort. During treatment, you may feel mild sensations such as warmth, tingling, or slight stinging depending on the procedure performed. After the treatment, some temporary redness, sensitivity, or mild soreness may occur, but these typically settle within a few days.
In most cases, active acne should be treated and brought under control before starting acne scar treatments. Ongoing breakouts can lead to new scars and may interfere with the effectiveness of scar treatments. Your dermatologist will usually first recommend treatments to manage the acne, and once the condition is stable, a personalised plan for treating the scars can be started.
The timeline for results varies depending on the type of treatment and the severity of the scars. Some treatments may show visible improvement within a few weeks, while others work by gradually stimulating collagen production in the skin, which can take several months to develop. In many cases, multiple treatment sessions are recommended to achieve the best results, with improvements becoming more noticeable over time.
Acne scars themselves typically do not become infected, because they are areas of healed skin. However, the surrounding skin can become infected if there is active acne, skin irritation, or damage to the skin. In some cases, infection may occur if acne scars are picked, scratched, or injured, or if the skin becomes infected after certain procedures without proper aftercare.
Seek Proper Dermatologist Care for Acne Scar Treatment
If you or your child are experiencing persistent or worsening acne scars, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in acne scar treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh