Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
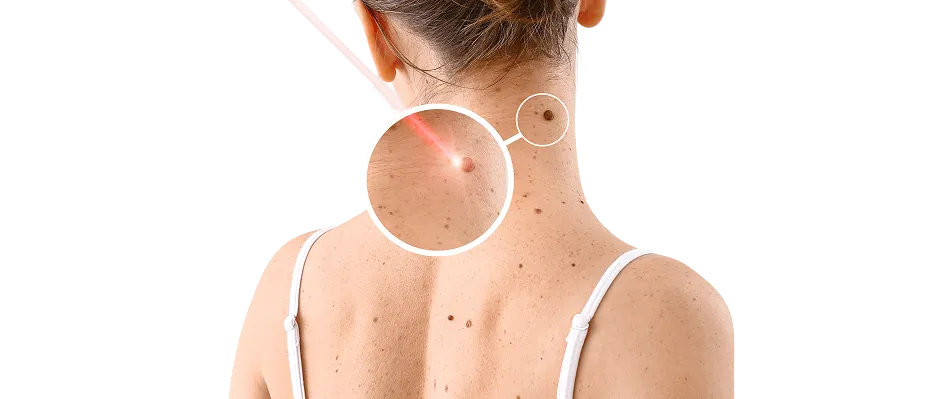
Mole removal is a specialised medical process focused on the safe, precise assessment and extraction of skin growths. Because moles, medically known as nevi, can range from benign cosmetic concerns to potential indicators of skin health issues, they often require professional evaluation to ensure both structural and diagnostic accuracy. While many moles are harmless, any lesion that shows changes in size, shape, or colour represents a shift in skin architecture that warrants clinical evaluation for health, comfort, or aesthetic peace of mind.
Moles can often be assessed and, when appropriate, removed safely through a dermatological approach. Treatment success relies on three core pillars: an accurate clinical diagnosis of the lesion's nature using dermatoscopy, a personalised selection of surgical or non-surgical removal techniques, such as shave excision, surgical excision, or punch biopsy, and consistent follow-up and monitoring when indicated to support skin health.




What Are Moles?
Moles are the result of cumulative clusters of melanocytes, the skin cells that produce pigment, growing together in a concentrated area. Most moles are benign skin lesions, though some may warrant monitoring or biopsy if they change. When the body's cellular growth patterns change, a mole may alter its border, symmetry, or pigmentation.
Mole removal is not simply a matter of cosmetic cleanup. It is a precise medical procedure involving the removal of the lesion and, in many cases, a laboratory analysis (pathology) to confirm the growth is healthy. Because these cellular changes can occur both on the surface and within the dermis, specialised dermatological care, using sterile surgical instruments and microscopic precision, helps guide the most appropriate removal method, with attention to diagnosis, wound healing, and scar outcomes.
What Are Common Types of Moles and When to Worry?
There are several distinct types of moles, and an accurate diagnosis by a dermatologist is essential because some lesions require immediate medical attention, while others are purely cosmetic. Most patients present with a variety of moles, which is why a comprehensive skin assessment is the standard of care.
Common Benign Nevi
These are the moles most people are familiar with, and they typically remain stable throughout a person's life.
-
Junctional Nevi
Typically brown or tan and flat or slightly raised; these are found at the junction of the epidermis and dermis. -
Compound Nevi
These contain melanocytes in both the epidermis and the dermis, often appearing raised and tan or light brown. -
Dermal Nevi
These are usually flesh-coloured, skin-toned, or light brown and are typically raised above the skin surface. They are very common as we age.
Atypical (Dysplastic) Nevi
These are moles that look different from common moles and may have irregular features.
-
Appearance
They are often larger, have irregular or notched borders, and feature a mix of colours (e.g., shades of tan, brown, or pink). -
Clinical Significance
While most atypical moles are benign, they can be associated with an increased risk of melanoma. If your dermatologist identifies an atypical mole, they may recommend monitoring, biopsy, or removal depending on its clinical features.
Congenital Nevi
These are moles that are present at birth or develop shortly thereafter.
-
Characteristics
They can range in size from small spots to large patches covering significant areas of the body. -
Clinical Significance
Larger congenital moles may carry a higher lifetime melanoma risk and often warrant regular dermatological follow-up.
Malignant Melanoma (The Red Flag Lesions)
It is critical to be vigilant for signs of malignancy. We use the ABCDE Rule as a primary guide for identifying suspicious changes:
-
Asymmetry
One half of the mole does not match the other. -
Border
The edges are irregular, ragged, notched, or blurred. -
Colour
The colour is not uniform; it includes shades of brown, black, blue, red, or white. -
Diameter
The spot is larger than 6mm (roughly the size of a pencil eraser). -
Evolving
The mole is changing in size, shape, colour, or is exhibiting new symptoms like itching, pain, or bleeding.
What Causes or Triggers Moles?
Moles, technically known as melanocytic nevi, are essentially clusters of melanocytes that have grown in a group rather than being spread evenly throughout the skin. Understanding why they form and what triggers changes in them is essential for both aesthetic management and long-term health surveillance.
Genetic Blueprint
Cumulative UV Exposure
Hormonal Fluctuations
Natural Ageing Process
Immune System Dynamics
Chronic Mechanical Irritation
How Are Moles Removed at TSN Dermatology?
Mole removal is a precise medical procedure performed with the dual goal of ensuring diagnostic accuracy and achieving the best possible cosmetic outcome. The medical term for a mole is a melanocytic nevus (plural: nevi), which forms when pigment cells called melanocytes aggregate in the skin.
While the majority of moles are benign, they may be removed for aesthetic reasons, physical comfort, or diagnostic health. Because skin cancers can sometimes be mistaken for common moles, it is vital that they are never casually removed before being examined by a doctor. Removing or destroying a suspicious lesion without proper assessment and histology may delay diagnosis and appropriate treatment. At TSN Dermatology, our specialists will evaluate your mole to determine the most appropriate treatment, explaining the benefits and risks of each technique to help you make an informed decision.
Individualised Treatment Approach
Our approach is tailored to your specific lesion and needs:
-
The Safety First Principle
If a mole appears atypical or suspicious, our priority is to remove it with a surgical margin to ensure the entire lesion can be analysed. -
Diagnostic Pathology
We will advise whether the removed tissue should be sent for histology (laboratory analysis) to definitively determine its character, whether it is benign or requires further medical intervention. -
Cosmetic Optimisation
For benign moles, we utilise surgical techniques that prioritise precision and minimal scarring.
Professional Removal Techniques
Our specialists determine the best approach based on the mole's size, depth, and clinical presentation:
-
Surgical Excision
This involves carefully cutting out the lesion, usually followed by fine, medical-grade stitches. This is a standard and commonly used technique when full-thickness removal is required. -
Shave Excision
A technique used for raised moles, where a specialised surgical blade is used to shave the top portion of the growth flush with the surrounding skin. This method typically results in a small, superficial wound that often heals without stitches, though healing time varies by site and individual. -
Laser Removal
In carefully selected lesions already assessed as benign, laser treatment may be considered in limited cases. Our specialists will assess whether this is appropriate for your specific mole.
The Pathology Process
Patient safety is our highest priority. Following removal, if your mole is sent for histological analysis:
-
Laboratory Examination
The tissue is examined under a microscope by a specialist to confirm its cellular structure. -
Definitive Diagnosis
This process confirms the nature of the mole, providing you with the necessary reassurance or, in rare cases, the information required for further treatment. -
Clear Communication
Our clinic team will contact you once the results are ready to discuss the findings, ensuring your long-term skin health is fully addressed.
Patient Preparation & Aftercare for Mole Removal
To support safe healing and the best possible cosmetic outcome, we have established clear guidelines for both before and after your procedure. Proper preparation helps minimise the risk of infection and complications, while disciplined aftercare is essential to support wound healing and help reduce the visibility of scarring.
Pre-Treatment Preparation: Getting Your Skin Ready
Your skin's condition on the day of the procedure is important for both safety and precision.
- Clean and Clear Skin
Please ensure the area to be treated is free of any creams, lotions, perfumes, or cosmetics. This is essential for maintaining a sterile surgical environment and ensuring clear visualisation of the lesion. - Medication Awareness
Please inform our team of all medications and supplements you are taking. If you are on blood-thinning medications or supplements (e.g., aspirin, fish oil, Vitamin E), we may advise you to stop them 3-5 days prior to your session to minimise the risk of bruising and bleeding during and after the procedure.
- Pause Active Skincare
For 3-5 days prior to your surgery, avoid using strong anti-ageing or exfoliating actives (like retinoids or chemical acids) on the area to be treated to prevent skin irritation. - What to Wear
Wear comfortable, loose-fitting clothing that allows easy access to the mole's location. Avoid tight fabrics that might rub against the treatment site immediately after the procedure.
Post-Treatment Aftercare: Supporting the Healing Process
Once your session is complete, your skin begins the process of tissue repair. Proper wound care is vital to prevent infection and ensure the best possible aesthetic outcome.
- Keep the Wound Clean and Dry
Follow your dermatologist's specific instructions regarding when you can shower and how to clean the site. Follow your dermatologist's instructions on when to clean or wet the site, as this can vary by procedure. - Managing Stitches and Dressings
If stitches were placed, keep the area covered with the provided dressing for the duration advised by your doctor. Do not submerge the wound in baths, swimming pools, or the ocean until the stitches are removed or the area has fully closed. - Do Not Pick or Scratch
As the wound heals, you may experience mild itching or a tight sensation. Do not pick or scratch at the healing site or any scabs that may form. Picking can disrupt the healing tissue, increase the risk of infection, and lead to more prominent or unsightly scarring.
- Strict Sun Protection
The new skin in the healing site is extremely sensitive to UV radiation. Once the dressing is removed, keep the scar protected with SPF 50+ sunscreen or a physical barrier (like a bandage or clothing) whenever you are exposed to the sun. UV rays can cause the new scar tissue to darken (hyperpigmentation), making it more visible. - Monitoring for Infection
While minor redness is normal, contact our clinic immediately if you notice signs of infection, such as:
- Increasing pain or swelling.
- The area feels hot to the touch.
- Persistent oozing, pus, or a foul odour.
- Spreading redness around the wound site.
- Consistency in Follow-up
If your procedure involves stitches, ensure you return for your scheduled removal session. Skipping this step can lead to stitch marks (track-mark scarring) if the sutures are left in for too long.



When Should You See a Dermatologist for a Mole?
You should consider seeking professional dermatological care if you notice any changes in the size, shape, or colour of an existing mole, if you discover a new growth that seems out of place, or if a lesion is causing you persistent discomfort or aesthetic concern.
While most moles are harmless, specialist evaluation is the most reliable way to ensure early detection of skin cancer and provide peace of mind. Seeking a clinical assessment is particularly important in the following scenarios:
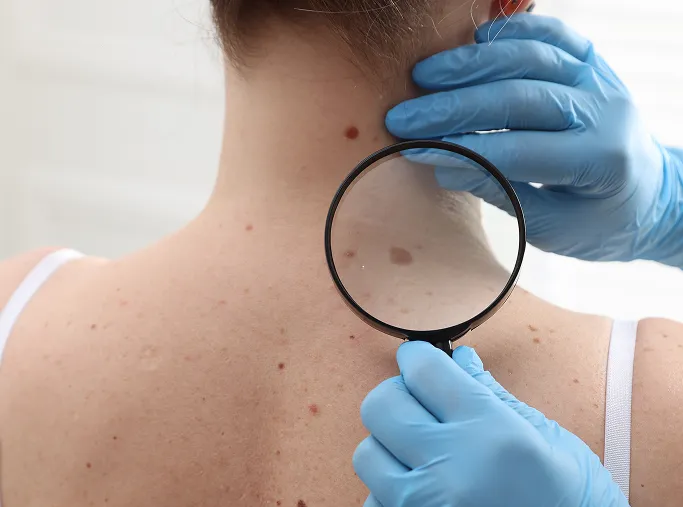
When You Notice the ABCDE Changes
If you notice any of these warning signs, it is important to have the mole assessed by a dermatologist. Early evaluation supports timely diagnosis and appropriate management.
When You Have a New Ugly Duckling
If you develop a new mole after the age of 30, or if you find a lesion that looks distinctively different or off compared to all your other moles, a dermatologist should evaluate it promptly.
When Moles Become Symptomatic
If a mole begins to itch, hurt, crust over, or bleed spontaneously without a clear external cause, this is a clinical red flag that requires an urgent dermatological check.
When Moles Are in High-Friction Areas
If you have moles located where clothing, jewellery, or daily activity causes constant rubbing, they may become chronically irritated. A dermatologist can assess these and recommend removal to prevent recurring inflammation or potential trauma.
If You Have a Personal or Family History
Individuals with a history of skin cancer, or those with a family history of atypical (dysplastic) nevi or melanoma, should be on a regular, proactive surveillance schedule.
When You Desire Professional Reassurance
If the appearance of a mole, regardless of its medical nature, is causing you anxiety or self-consciousness, a clinical assessment can provide professional clarity. We can confirm if the mole is benign and discuss removal options if it is causing you aesthetic distress, ensuring you are supported through the entire process.
FAQs About Mole Removal
Usually, yes. Once a mole is removed, it often does not return, although some lesions can recur if residual cells remain.
We prioritise your comfort by using effective local anaesthesia. You will receive a small injection to numb the area, which ensures that you feel little to no pain during the procedure itself—only slight pressure. Once the anaesthetic wears off, you may experience mild tenderness, which can often be managed with simple pain relief if needed.
No. We strongly advise against using any over-the-counter mole removal kits or home remedies. These methods can cause severe chemical burns, permanent scarring, or infection. Furthermore, they destroy the tissue, making it impossible to perform a pathology examination, which is essential to rule out skin cancer. Always have a mole professionally assessed by a dermatologist first.
Any procedure that involves cutting the skin will leave some form of a mark. However, our dermatologists are trained in precise surgical techniques to help scars heal as discreetly as possible.
There is no strict limit, but we typically limit the number of removals per session to ensure your comfort and allow for proper post-procedure healing. During your consultation, we can assess all your moles and create a safe, manageable schedule for removal if you have multiple areas of concern.
Expert Dermatologist Care for Mole Removal
If you are concerned about moles or wish to have them safely removed, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can assess your skin and develop an effective, personalised treatment plan focused on safe removal while supporting long-term skin health and optimal cosmetic results. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in mole removal, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh