Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
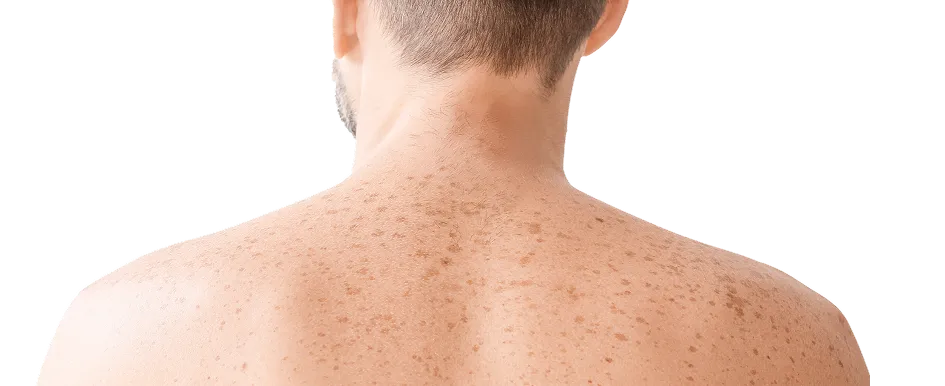
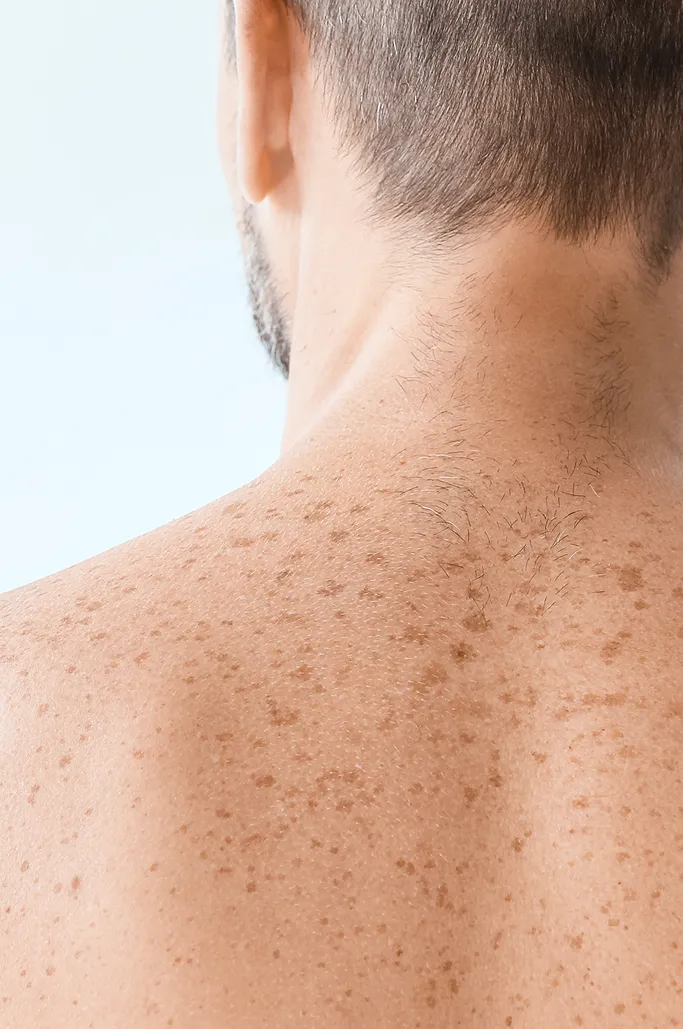
Skin pigmentation disorders are a common dermatological concern affecting individuals of all skin types. They are characterised by changes in skin colour, manifesting as dark patches (hyperpigmentation) or light spots (hypopigmentation), which can be caused by sun damage, hormonal fluctuations, inflammation, or genetic factors. While these changes are often benign, they can significantly affect an individual's self-esteem and daily confidence.
Although some forms of pigmentation can be persistent, they can be effectively managed with proper diagnosis, personalised treatment, and long-term dermatological care under the guidance of a specialist.




What Is Skin Pigmentation?
Skin pigmentation is usually due to an increase in melanin pigment (hyperpigmentation) in the skin. Melanin is a natural pigment that gives colour to our skin and hair. Pigment-producing cells, known as melanocytes, can sometimes be activated or triggered to produce excessive amounts of melanin pigment, leading to visible pigmentation problems.
Some of the common triggers for this process include skin injury, ultraviolet (UV) radiation from sunlight, and hormonal fluctuations. It is important to recognise that not all brown spots on the face are the same; different conditions involve different depths and causes, and therefore require different forms of specialised medical treatment. Pigmentation is not simply a cosmetic issue—it is a complex medical condition involving cellular regulation that often requires professional dermatological assessment for effective and safe control.
What Are Common Types of Skin Pigmentation?
There are several distinct types of pigmentation, and an accurate diagnosis is essential as each condition requires a specific medical approach. Our dermatologists will map the affected areas to determine the best treatment strategy.
Freckles and Lentigines
-
Freckles
These are small, light brown marks that appear more frequently in individuals with fair skin. They are most common on sun-exposed areas like the nose and cheeks, and tend to become darker with sun exposure. While they may lighten with consistent sun protection, they often require active management if cosmetic improvement is desired. -
Lentigines
Often called age spots, these are brown patches resulting from cumulative sunlight exposure. They are more common in people above 40 and can be found on the face and the back of the hands in both fair and dark complexions. Unlike freckles, lentigines usually do not fade with sun protection alone; if treatment is desired, laser therapy or cryotherapy may be used.
Hori's Nevus (Naevus of Hori)
-
Characteristics
This condition involves a collection of pigment cells (melanocytes) located deep within the skin. It typically presents as small, round, brown or slate-grey spots on the cheeks. -
Demographics
It is most commonly seen in Asian women between the ages of 30 and 50. -
Treatment
Addressing Hori's nevus usually requires a series of laser sessions (typically at least four). It is important to note that laser treatment may initially cause temporary post-inflammatory hyperpigmentation, but this will gradually settle over time as the skin heals.
Melasma
-
Characteristics
Melasma presents as light to dark brown, often symmetrical patches on the cheeks, forehead, nose, or chin. -
Demographics
It is significantly more common in women, typically appearing between the ages of 20 and 40. -
Contributing Factors
Multiple factors contribute to its formation, including chronic sun exposure, hormonal changes (such as pregnancy, menopause, or the use of oral contraceptive pills), and a genetic predisposition. -
Treatment Strategy
Because melasma is a complex, chronic condition, management often involves a multi-modal approach:
Lightening Creams: Customised combinations of hydroquinone, retinoids, mild steroids, and Vitamin C.
Oral Medications: Such as tranexamic acid to help manage pigment production.
Clinical Procedures: Chemical peels or specialised laser therapies.
-
Maintenance
It is critical to avoid excessive sun exposure and use a high-performance, broad-spectrum sunscreen consistently to prevent melasma from recurring after treatment.
Common Symptoms of Skin Pigmentation to Look Out For
As pigmentation disorders can originate in different layers of the skin—the epidermis (surface) or the dermis (deeper layer)—they often present with distinct visual and textural markers. Recognising these specific signs helps distinguish between common pigmentary changes and those requiring clinical intervention.

Characterised by Depth and Pigment Type
-
Epidermal Pigmentation
Typically appears as well-defined, light-to-medium brown patches with a sharp border. These often respond more readily to topical lightening agents and superficial peels (e.g., most solar lentigines and epidermal melasma). -
Dermal Pigmentation
Appears as hazy, slate-grey, or bluish-brown patches with poorly defined or fuzzy borders. These are located deeper in the skin and often require targeted laser therapy rather than surface creams (e.g., Hori's nevus and dermal melasma).
The Pattern of Pigmentation
-
Symmetrical Distribution
A hallmark of hormonal conditions like melasma. You may notice matching brown or grey-brown patches on both sides of the face, particularly across the cheeks, bridge of the nose, forehead, and upper lip. -
Sun-Exposed Clustering
Common in solar lentigines, these appear as scattered, individual brown spots localised specifically to areas that have received the most sun exposure over your lifetime—the bridge of the nose, the tops of the cheeks, the backs of the hands, and the décolletage. -
Inflammatory Footprints
In Post-Inflammatory Hyperpigmentation (PIH), the dark marks follow the exact shape and size of a previous injury, such as a resolved acne nodule, a scratch, or an area where a rash once existed.
Symptoms Requiring Urgent Dermatological Check
Beyond the cosmetic appearance, certain evolutionary signs indicate that the pigment cell biology has changed, which necessitates an immediate professional biopsy to rule out malignancy:
-
The Ugly Duckling Lesion
A single spot that looks dark, jagged, or multi-colored compared to all your other moles or freckles. -
Spontaneous Surface Changes
A pigmented spot that develops a crust, begins to bleed, ulcerates, or scabs over without a history of physical injury. -
Rapid Evolution
A spot that is actively growing in size or changing colour month-over-month.
Visible Structural Changes
-
Orange Peel Texture
Occasionally, dense pigmentation like seborrheic keratoses (which can be mistaken for age spots) will have a slightly raised, waxy, or stuck-on appearance with a rougher, velvety texture compared to the surrounding skin. -
Lack of Bleaching Response
A key diagnostic symptom is that the pigment does not turn white when you press on it (blanching). If you press your finger firmly on a spot and the colour remains dark, the pigment is located deep in the tissue rather than being a result of dilated blood vessels (like redness).
What Causes or Triggers Skin Pigmentation?
Pigmentation problems arise when the skin's melanin-producing cells, known as melanocytes, become overactive or are triggered to produce excessive amounts of pigment. While the underlying cause often involves a mix of genetics and biology, specific external and internal triggers frequently activate these cells, leading to visible dark spots or patches.
UV Radiation from Sunlight
Medications and Photosensitivity
Genetic Predisposition
Hormonal Fluctuations
Skin Injury and Inflammation
Whenever the skin is injured, it initiates a complex healing response. In many individuals, this process causes the nearby melanocytes to go into overdrive, leaving behind a dark mark long after the initial wound has healed. This is known as Post-Inflammatory Hyperpigmentation (PIH) and is commonly triggered by:
- Inflammatory acne (cysts and nodules).
- Eczema or contact dermatitis flare-ups.
- Physical trauma, such as aggressive skin scrubbing or accidental scratches.
- Post-procedure inflammation from laser treatments if the skin is not properly prepped or protected.
Environmental Pollutants
How is Skin Pigmentation Treated at TSN Dermatology?
Effective management of skin pigmentation requires a strategic approach. Because pigmentation often resides at different depths—superficial (epidermal) or deep (dermal)—we frequently utilise a combination of clinical modalities to achieve optimal results. Treatment plans are tailored to your specific skin type and the nature of the pigmentation to ensure both safety and efficacy.

Individualised Treatment Approach
Pigmentation varies significantly based on its origin, your skin tone, and your lifestyle. A one-size-fits-all approach is rarely successful and can sometimes worsen pigment. Our treatment plans are customised based on:
Pigmentation Classification
Distinguishing between epidermal, dermal, or mixed types.
Skin Tone & Sensitivity
Selecting technologies that are safe for your specific skin type to minimise the risk of post-inflammatory hyperpigmentation (PIH).
Lifestyle & Downtime
Balancing the intensity of treatment with your daily schedule.
Maintenance Requirements
Planning for long-term care to prevent the pigment from returning.
Topical Treatments and Depigmenting Agents
Topical treatments are the cornerstone of managing pigmentation, particularly for conditions like melasma.
Active Brightening Creams: We prescribe pharmaceutical-grade agents—including hydroquinone, retinoids, kojic acid, and Vitamin C—to inhibit melanin production and accelerate skin cell turnover.
Maintenance Maintenance: For long-term control, we may transition you to non-hydroquinone brightening agents to maintain results safely.
Sun Protection: A rigorous, daily broad-spectrum SPF 50+ regimen is non-negotiable. Without it, the melanin-producing cells will continue to react to UV light, rendering other treatments ineffective.
Laser and Light Therapies
For stubborn, deep-seated, or extensive pigment, we employ advanced medical lasers designed to shatter melanin clusters without damaging the surrounding skin.
Q-Switched and Picosecond Lasers: These are our gold standard technologies for breaking down deep-seated pigment like Hori's nevus and solar lentigines. They work by delivering energy in extremely short pulses, which fragments the pigment into smaller particles that the body can naturally clear away.
Tailored Sessions: We will determine the appropriate frequency for your laser sessions, allowing sufficient time for the skin to heal and the pigment to fade between treatments.
Chemical Peels
Pharmaceutical-grade chemical peels are generally effective for exfoliating the top layers of the skin to remove superficial pigment.
Surface Resurfacing: By controlled removal of the skin's outer layer, we can significantly fade sun spots, freckles, and surface-level melasma.
Controlled Depth: We select the peel strength based on your skin type and the desired outcome, ensuring the process is safe while maximising brightness and texture improvement.
Systemic Therapies
For recalcitrant conditions like melasma that do not respond to topicals and lasers alone, we may consider oral medications.
Tranexamic Acid: This oral medication is frequently used to manage chronic or recurrent melasma by reducing the vascular and inflammatory components that trigger melanocyte activity. It is prescribed under specialist supervision with regular monitoring to ensure your safety.
Tips on Daily Care and Prevention of Skin Pigmentation
Effective management of skin pigmentation is as much about protecting the results you achieve in the clinic as it is about the treatments themselves. Because melanocytes are highly reactive cells, consistent daily habits are required to prevent existing spots from darkening and to stop new ones from forming.
Strict Sun Protection
Daily, broad-spectrum SPF 50+ sunscreen is the most important treatment for pigmentation. UV radiation is the primary trigger that keeps melanocytes overactive.
-
Beyond the Face
Ensure you apply sunscreen to the neck, décolletage, and backs of the hands. -
Physical Barriers
When outdoors in Singapore's tropical sun, a wide-brimmed hat and seeking shade are your best defences against UV-induced pigment reactivation.
Gentle Cleansing and Skincare
Avoid harsh scrubs, loofahs, or aggressive sonic brushes, as they can cause micro-inflammation in the skin, which triggers PIH (Post-Inflammatory Hyperpigmentation).
-
Stick to the Basics
Use a mild, pH-balanced, fragrance-free cleanser to keep your skin barrier intact and calm.
Early Intervention for Skin Inflammation
Pigmentation is often an aftermath of inflammation. If you have an acne breakout, eczema flare, or skin irritation, treat it early and effectively. The faster you resolve the inflammation, the less likely it is that the area will be left with a dark, stubborn mark.
Avoidance of Irritant Triggers
Identify your personal triggers. For many patients, certain essential oils, fragrances in skincare, or even prolonged heat exposure can act as low-grade irritants that keep pigmentation active. When in doubt, simplify your routine to non-comedogenic and hypoallergenic products.
Consistency with Brightening Topicals
If you have been prescribed a home-care regimen (such as hydroquinone or retinoids), consistency is vital. These products work by suppressing the pathways that produce excess melanin; stopping and starting prevents the skin from achieving a stable, even tone. Always follow your dermatologist's specific instructions regarding application frequency.



When Should You See a Dermatologist for Skin Pigmentation?
While many forms of pigmentation are benign, they can be persistent and difficult to treat without medical oversight. You should consider seeking professional dermatological care if you notice unexpected changes in your skin tone, if you are experiencing persistent dark spots that do not fade with standard skincare, or if a lesion displays signs of atypical growth. Specialist care is particularly important in the following scenarios:

When Pigment Changes in Appearance (The ABCDEs)
If a pigmented spot begins to change in size, shape, colour (becoming multi-coloured), or starts to itch, bleed, or crust over, it requires an immediate clinical assessment. These can be red flags for skin cancer rather than simple pigmentation.
When OTC Products Fail
If you have been using brightening serums or exfoliating acids for several months without seeing an improvement in the appearance of your spots, the pigment may be dermal (deeper). This requires professional-grade diagnostics to identify the depth and specific type of pigment.
When You Desire Tangible Results
Pigmentation treatments—especially for complex conditions like melasma or Hori's nevus—are a significant investment of time and resources. A dermatologist can provide a realistic roadmap, preventing the frustration of ineffective, trial-and-error home remedies.
If You Have a History of Inflammation
If you notice that even minor acne breakouts, insect bites, or minor scrapes consistently leave behind long-term dark marks (PIH), a dermatologist can provide a proactive management plan to calm the inflammation and prevent the pigment from setting in.
When Pigmentation Impacts Your Confidence
Pigmentation, particularly on the face, can significantly impact quality of life and self-esteem. Professional treatment not only aims to clear the skin but also provides the psychological reassurance that the condition is being managed safely and effectively.
FAQs About Skin Pigmentation
Many forms of pigmentation, especially chronic conditions like melasma or Hori's nevus, are prone to recurrence. While we can achieve significant improvement and clear visible spots, curing the underlying biological tendency for pigment production is difficult. Most patients achieve excellent results with a combination of active treatment and a long-term maintenance plan.
When prescribed by a dermatologist at the appropriate strength and used as part of a structured treatment roadmap, brightening creams are safe and effective. Problems typically arise from unsupervised, prolonged use or the application of miracle creams purchased online that may contain harmful, unregulated ingredients. We monitor your progress closely to ensure your skin health is never compromised.
Modern laser technology, such as Picosecond lasers, is generally effective for various skin types. However, settings must be carefully calibrated for patients with deeper or darker skin tones, as overly aggressive laser settings can actually trigger more pigment (Post-Inflammatory Hyperpigmentation). An initial consultation allows us to assess your specific skin type and select the safest, most effective modality for you.
Most common forms of pigmentation (like freckles or sun spots) are benign. However, certain skin cancers can mimic the appearance of common brown spots. This is why it is critical to have any new or changing spot professionally examined by a dermatologist using dermatoscopy rather than attempting to treat it at home.
Seek Proper Dermatologist Care for Skin Pigmentation
If you or your child are concerned about uneven skin tone or pigmentation, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help you better understand your skin and explore personalised treatment options to improve clarity and overall skin appearance. For more information or to book an appointment, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in skin pigmentation treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh