Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
Dandruff, also known as seborrhoeic dermatitis or pityriasis capitis, is a common inflammatory condition that affects both children and adults. It is characterised by persistent itching, redness, and flakiness on the scalp, which can sometimes extend onto the face, ears, and body. In infants, it can present as cradle scalp. While dandruff cannot be permanently cured, it can be effectively controlled with appropriate treatment and consistent scalp care.




What Is Dandruff?
Dandruff occurs when the scalp sheds skin cells more rapidly than usual, often accompanied by mild inflammation. This process is linked to a combination of factors, including oil (sebum) production and sensitivity to Malassezia yeast.
Dandruff is not simply a result of poor hygiene. It is a complex medical condition involving skin barrier dysfunction and immune response, which is why specialised dermatological care is often required for effective control and the prevention of recurrence.
What Are Common Types of Dandruff?
While we often group all scalp flaking under the label of dandruff, there are different clinical presentations of seborrhoeic dermatitis that may affect the scalp and surrounding areas. Accurate diagnosis is important, as each may require slightly different management strategies.
Pityriasis Capitis (Classic Dandruff)
- This is the most common form. It is characterised by fine, white or greyish flakes on the scalp.
- It is usually caused by an inflammatory reaction to Malassezia yeast and is often accompanied by mild itching.
Infantile Seborrhoeic Dermatitis (Cradle Cap)
- Commonly seen in infants, this presents as thick, crusty, yellowish patches on the scalp.
- While it can look alarming to parents, it is a self-limiting condition that typically responds well to gentle, appropriate cleansing and moisturising.
Seborrhoeic Dermatitis (Inflammatory Type)
- This is a more intense presentation that involves both flaking and distinct redness.
- It often occurs in oil-rich areas beyond the scalp, such as the eyebrows, sides of the nose (nasolabial folds), the skin inside or behind the ears, and sometimes the chest.
- The flakes here are often yellowish and greasy in appearance.
Seborrhoeic Dermatitis in Adults (Body/Fold Involvement)
- In some cases, the inflammation extends to other areas of the body rich in sebaceous glands, such as the chest, eyebrows, sides of the nose, behind the ears, and occasionally skin folds.
- In these areas, it appears as red, symmetrical, and sometimes itchy patches.
Common Symptoms of Dandruff to Look Out For
Dandruff symptoms can vary in intensity, often shifting between periods of relative calm and noticeable flare-ups. While the presentation is unique to each individual, the following signs are commonly associated with the condition:
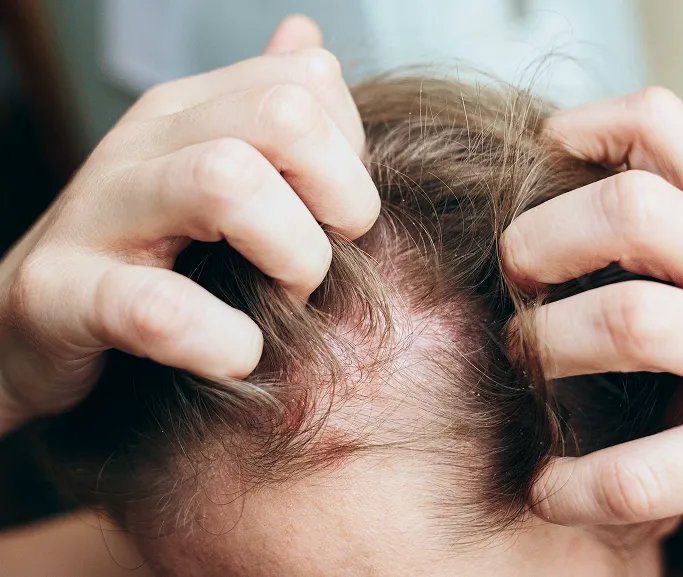
Persistent Scalp Itching
Visible Flaking
Redness and Inflammation
Greasy or Waxy Scales
Tenderness and Burning
Extension Beyond the Scalp
What Causes or Triggers a Dandruff Flare-up?
Dandruff flare-ups often occur when the balance of the scalp environment is disturbed, allowing the Malassezia yeast to thrive and trigger an inflammatory response. While the specific triggers differ from person to person, the following factors are commonly recognised as contributors to recurring symptoms:
Weather and Seasonal Changes
Stress
Product Build-up and Harsh Chemicals
Infrequent Cleansing
Hormonal Fluctuations
How Is Dandruff Diagnosed?
While dandruff is often managed with over-the-counter shampoos, an accurate diagnosis is important to rule out other skin conditions, such as psoriasis, fungal infections, or eczema, that may mimic dandruff but require different treatment approaches. A dermatologist may assess your scalp using the following methods:
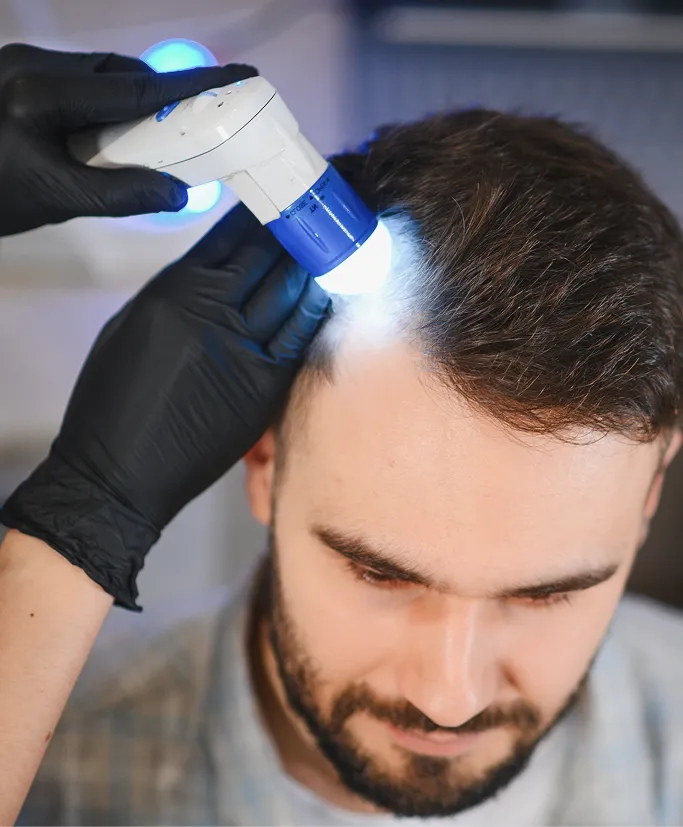
Clinical Examination
Medical History Review
Assessment of Symptom Distribution
Exclusion of Other Dermatological Conditions
Dandruff can be easily confused with other conditions. A dermatologist is trained to differentiate between:
-
Scalp Psoriasis
Characterised by thicker, silvery-white plaques that may be more defined than dandruff flakes. -
Fungal Infections (Tinea Capitis)
More common in children, these may cause patchy hair loss or brittle, broken hairs. -
Contact Dermatitis
Often identified by a history of recent changes in shampoos, dyes, or styling products that triggered the reaction.
Skin Scrapings or Laboratory Tests
How is Dandruff Treated at TSN Dermatology?
Effective management of dandruff (seborrhoeic dermatitis) requires a strategy that balances anti-fungal action, inflammation control, and long-term scalp barrier maintenance. Because symptoms vary, we provide personalised care plans tailored to your specific scalp needs.
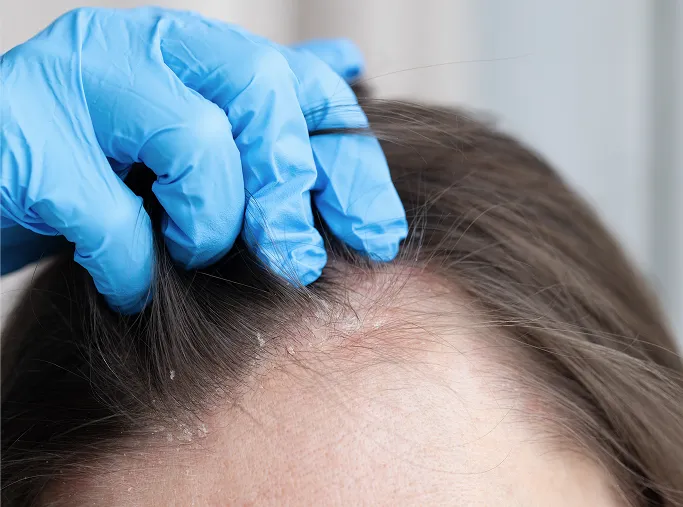
Individualised Treatment Approach
As dandruff severity ranges from mild, occasional flaking to persistent, inflammatory patches that affect the face and ears, treatment is never one-size-fits-all. Our approach is based on:
Diagnosis Confirmation
Ruling out conditions like scalp psoriasis or fungal infections that require different medications.
Severity of Inflammation
Assessing the degree of redness, scaling, and whether the rash has spread to non-scalp areas.
Lifestyle Factors
Identifying hair care habits, product sensitivities, and environmental triggers that contribute to flare-ups.
Long-term Maintenance
Establishing a sustainable scalp-care routine to prevent yeast overgrowth and keep symptoms in remission.
Medicated Shampoos
Medicated shampoo is the primary tool for managing dandruff. Unlike cosmetic shampoos, these are formulated to target the root causes of flaking:
Anti-fungal Agents: These help reduce the population of Malassezia yeast on the scalp.
Anti-inflammatory Ingredients: These soothe redness and help reduce itching and inflammation.
Keratolytic Agents: These help lift and remove stubborn, waxy scales so the scalp can heal.
Guidance: We provide specific instructions on contact time, how long to leave the lather on your scalp, to ensure the active ingredients are fully effective.
Topical Treatments
For patients experiencing significant inflammation beyond the scalp (such as around the eyebrows, nose, or behind the ears), topical therapy is essential.
Medicated Lotions and Creams: We may prescribe steroid or non-steroidal formulations to quickly calm intense itching and redness in sensitive skin areas.
Scalp Solutions: For severe scalp scaling that doesn't respond to shampoo alone, specialised scalp lotions can be applied directly to the skin to speed up barrier repair.
Systemic Treatments for Severe Cases
In instances where dandruff is extensive, persistent, or resistant to topical treatments, systemic therapy may be considered.
Oral Anti-fungal Medications: These are reserved for severe, treatment-resistant cases. These medications work from within to control the Malassezia population and require periodic monitoring by our specialists to ensure safety and effectiveness.
Tips on Daily Dandruff Care and Flare Prevention
Maintaining a healthy scalp requires more than just picking up an anti-dandruff shampoo. Consistent care habits help control the yeast populations that trigger inflammation, reduce scalp irritation, and prevent the return of visible flaking.
Gentle Cleansing and Scalp Hygiene
-
Consistent Shampooing
Regular cleansing is vital to remove excess oil (sebum) and dead skin cells. If you have a dry scalp, aim for every other day; for oilier scalps, daily washing may be necessary to keep yeast activity in check. -
Proper Application
When using medicated shampoos, focus the product on the scalp rather than just the hair. Gently massage it in and, most importantly, let it sit on the scalp for 5 to 10 minutes before rinsing. This contact time is what allows the active ingredients to effectively neutralise the Malassezia yeast. -
Lukewarm Water
Avoid washing with hot water, which can strip the scalp of its natural barrier and trigger inflammatory flare-ups.
Managing Product Use
-
Minimise Build-up
Avoid heavy styling gels, waxes, or pomades, as these create a breeding ground for yeast. If you must use products, ensure you are washing your hair thoroughly at the end of the day. -
Fragrance-Free Choices
If your scalp is prone to irritation, switch to fragrance-free or hypoallergenic hair products to reduce the risk of contact dermatitis, which can mimic or worsen dandruff.
Lifestyle and Environmental Factors
-
Stress Management
Since emotional stress can trigger flares, finding ways to manage tension is a practical component of scalp health. -
Sun Exposure
Avoid excessive heat and irritation to the scalp, as these can worsen inflammation.
Early Management of Flares
-
Stay Proactive
Do not wait for a full-blown flare-up to start your treatment. If you notice a slight increase in itching or flakiness, resume your prescribed medicated shampoo regimen immediately to get ahead of the inflammation. -
Avoid Scratching
Scratching damages the skin barrier and can lead to secondary bacterial or fungal infections. Keep your fingernails short and try to soothe the itch with medicated lotions if recommended by your dermatologist.
Environmental Control
-
Monitor Local Conditions
In Singapore's hot and humid climate, scalp sweat is inevitable. Try to shower shortly after intense exercise or being outdoors for long periods to prevent sweat and oils from lingering on the scalp.



When Should You See a Dermatologist for Dandruff?
While mild flaking can often be managed with consistent use of over-the-counter medicated shampoos, there are times when self-treatment is insufficient. Persistent scalp concerns can sometimes indicate a more complex condition that requires prescription-strength intervention. You should schedule a consultation with a dermatologist if you experience any of the following:
Inadequate Relief from OTC Products
If you have used active-ingredient shampoos (such as those containing zinc pyrithione, ketoconazole, or selenium sulfide) as directed for 4 to 6 weeks without a noticeable reduction in flaking or itching, you may need a prescription-strength antifungal or anti-inflammatory topical.
Signs of Secondary Infection
If you notice crusting, oozing, pus, or if your scalp feels painful to the touch, this may indicate a bacterial or severe fungal infection that requires medical clearance.
Severe Scaling or Plaque Formation
If the scales on your scalp feel thick, raised, and silvery—or if they extend well beyond your hairline onto your forehead, ears, or neck—it may be scalp psoriasis rather than dandruff. These conditions require different, often more intensive, management strategies.
Itching That Disrupts Daily Life
If the itch is so persistent that it impacts your sleep, ability to concentrate, or social confidence, a dermatologist can provide advanced treatments to calm the inflammation and restore comfort.
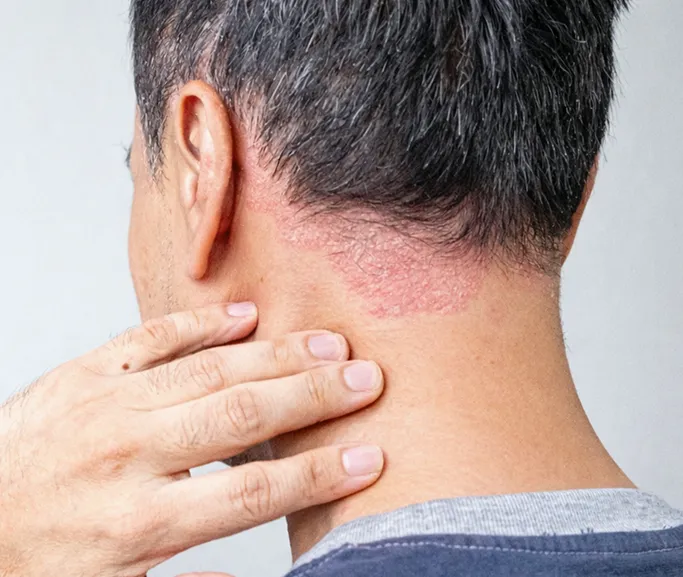
Rash Spread to Other Areas
If the flaking or redness starts appearing on your face (specifically the eyebrows, nasal folds, or ears) or your upper body, this is a clear sign that the condition is spreading and requires professional control to prevent further discomfort.
Hair Loss or Breakage
If you notice patches of hair thinning, bald spots, or hair that seems to be breaking off near the root, you must rule out conditions like tinea capitis (scalp ringworm), which needs specific medical treatment to prevent permanent hair follicle damage.
FAQs About Dandruff
No. Dandruff (seborrhoeic dermatitis) is not contagious. It is an inflammatory reaction to the presence of Malassezia yeast, which is naturally present on everyone's skin. You cannot catch dandruff from others, nor can you spread it through physical contact or sharing personal items like combs or hats.
Dandruff is highly manageable, and with consistent use of the right medicated shampoos and appropriate scalp care, most patients can successfully clear the flaking and keep the condition in remission. However, there is no permanent cure for it.
Yes, when used according to a dermatologist's instructions. While some people worry about harsh ingredients, medicated shampoos are formulated to treat the scalp without damaging the hair. We typically recommend using the medicated shampoo once or twice a week to prevent flares while using a gentle, daily shampoo in between.
Not exactly. While they look similar, dandruff is specifically linked to an overgrowth of yeast and inflammation in oil-rich areas. Dry skin is simply a lack of moisture. This is why using heavy moisturisers or oils on a dandruff-prone scalp can sometimes worsen scalp scaling or irritation in some individuals.
Dandruff itself does not cause hair loss, but the scratching associated with it can. Vigorous scratching can damage hair follicles and cause physical hair breakage. If you notice actual hair thinning or bald patches, it is important to see a dermatologist, as this may indicate a different scalp condition, like a fungal infection or alopecia.
Seek Proper Dermatologist Care for Dandruff
If dandruff is ongoing or getting worse for you or your child, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in dandruff treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh