Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
Eczema is a chronic inflammatory skin condition that affects both children and adults. It is characterised by persistent itching, dry and inflamed skin, and recurrent flare-ups that can significantly affect daily comfort, sleep, and quality of life. The most common type of eczema is atopic dermatitis.
Although eczema cannot be permanently cured, it can be effectively managed with proper diagnosis, personalised treatment, and long-term skin care under the guidance of a dermatologist.



What Is Eczema?
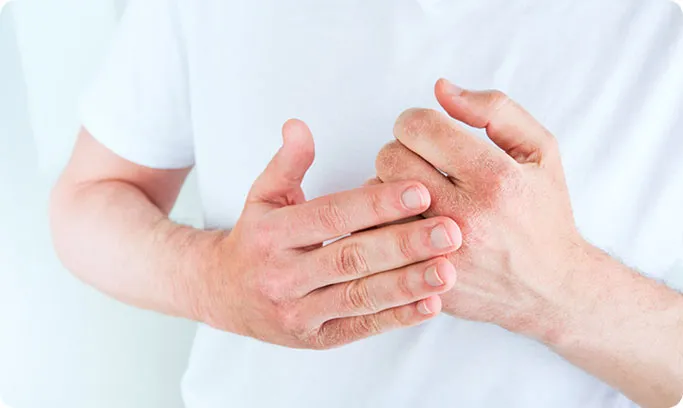
Eczema is a condition in which the skin barrier does not function properly, making the skin more sensitive to irritants, allergens, and environmental triggers. This impaired barrier allows moisture to escape easily and increases inflammation within the skin, leading to itchiness, redness, and recurrent rashes.
Eczema is not simply dry skin. It is a complex medical condition involving immune system overactivity and skin barrier dysfunction, which is why specialised dermatological care is often required for effective control.
What Are Common Types of Eczema?
There are several types of eczema, and accurate diagnosis is important for appropriate treatment.
Atopic Dermatitis
- A very common form of eczema, affecting up to 20% of children in Singapore, often beginning in early childhood.
- Typically presents as an itchy rash on the neck and folds of the limbs, and is frequently associated with asthma, allergic rhinitis, or allergic conjunctivitis.
- Has a genetic basis and may significantly affect sleep, school performance, and self-esteem in more severe cases.
Seborrhoeic Dermatitis
- Presents as a red, flaky rash affecting oil-rich areas such as the scalp, face, and ears, and may extend to the chest, armpits, or groin.
- Occurs in both infants and adults, with symptoms that may fluctuate or recur over time.
- Thought to be related to an inflammatory reaction to Malassezia, a yeast that normally resides on the skin.
Nummular (Discoid) Eczema
- Characterised by round or coin-shaped patches that commonly appear on the limbs and sometimes the trunk.
- The rash is often intensely itchy and may be dry and scaly, or oozy and crusted when inflamed.
- Dry skin is a common contributing factor, and lesions may persist or recur without appropriate treatment.
Dyshidrotic Eczema (Pompholyx)
- Causes intensely itchy, small fluid-filled blisters on the palms, sides of the fingers, soles, or toes.
- Blisters may recur and can leave the skin dry, cracked, or painful after they resolve.
- Flare-ups may be triggered by heat, sweating, stress, or contact allergens.
Contact Dermatitis
- Develops when the skin comes into contact with an irritant or allergen, resulting in a red, itchy rash.
- May present with swelling, blistering, scaling, or dryness depending on the severity of exposure.
- Identification of the trigger is key, and patch testing may be recommended in suspected allergic contact dermatitis.
Asteatotic Eczema
- Also known as xerotic eczema, this condition results from excessive skin dryness and is more common in older individuals.
- Commonly affects the legs and sides of the trunk, appearing as dry, cracked, scaly, and itchy skin.
- Cold or low-humidity environments can trigger flare-ups, making regular moisturisation important.
Stasis Dermatitis
- Associated with venous insufficiency or varicose veins affecting blood circulation in the lower legs.
- Presents as red, scaly, dry or weepy patches on the lower legs, often accompanied by swelling.
- May lead to brown pigmentation and skin thickening over time if the underlying condition is not managed.
Neurodermatitis (Lichen Simplex Chronicus)
- Results from repeated scratching or rubbing of a localised area of skin.
- Appears as a thickened, leathery, and intensely itchy patch, commonly affecting the neck, wrists, ankles, or genital region.
- The itch-scratch cycle can be difficult to break and often worsens during periods of stress.
Common Symptoms of Eczema to Look Out For
Eczema can present differently from person to person, and symptoms may fluctuate between periods of flare-ups and remission. While the severity varies, the following are some of the most common signs and features patients may experience.
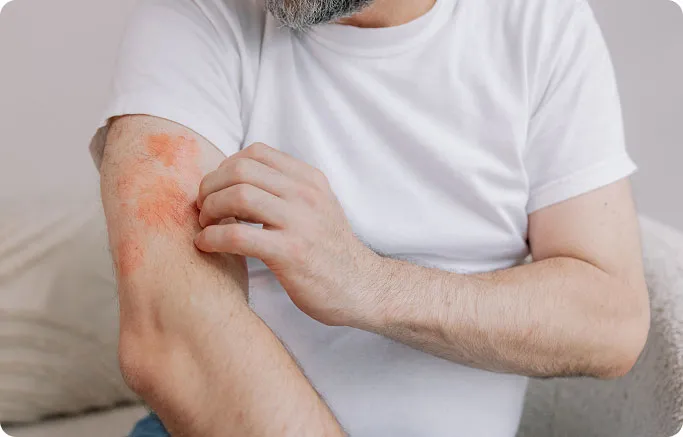
Persistent Itching
Ongoing itch is a hallmark symptom of eczema and may range from mild to severe, sometimes disrupting sleep and daily activities during flare-ups.
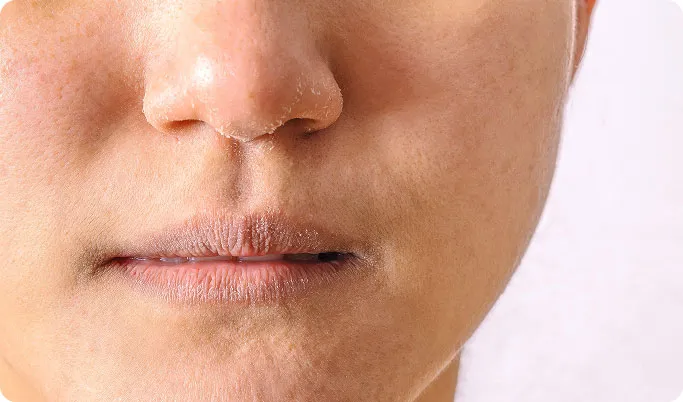
Dry Or Rough Skin
The skin may feel dry, tight, or rough due to a weakened skin barrier, making it more prone to irritation and sensitivity.
Redness And Inflammation
Affected areas often appear red and inflamed, reflecting active irritation within the skin.
Scaly Or Cracked Patches
The skin may become flaky, scaly, or develop painful cracks, particularly in areas exposed to friction or dryness.
Oozing Or Crusting During Acute Flares
In more inflamed episodes, small blisters or raw areas may ooze fluid and form crusts.
Thickened Skin In Long-Standing Cases
Chronic scratching or rubbing can cause the skin to become thickened and leathery over time (a process known as lichenification).
What Causes or Triggers an Eczema Flare-up?
Eczema flare-ups can occur when the skin barrier is disrupted or exposed to certain environmental or lifestyle factors. Triggers vary between individuals, but the following are commonly recognised contributors.
Heat And Humidity
Soaps, Detergents and Fragrances
Dust Mites and Environmental Allergens
Stress
Sweat and Friction
Certain Fabrics
How Is Eczema Diagnosed?
Accurate diagnosis is important, as several other skin conditions can mimic eczema and require different treatments. A dermatologist may assess eczema using the following methods:
Clinical Examination
Medical History Review
Assessment of Symptom Pattern and Triggers
Skin Scrapings or Lab Tests
Patch Testing
Exclusion of Other Skin Conditions
How is Eczema Treated at TSN Dermatology?
Effective eczema management requires an individualised treatment plan tailored to the severity of the condition, patient age, trigger factors, and lifestyle.

Individualised Treatment Approach
As eczema varies greatly from person to person (with some patients experiencing mild, occasional flares, while others have chronic or severe disease that affects daily functioning and sleep), treatment must be customised to the individual in order to be effective. Treatment plans are tailored based on:
Type of eczema diagnosed
Extent and location of skin involvement
Frequency and severity of flare-ups
Impact on quality of life
Age and medical history of the patient
Regular follow-up allows treatment to be adjusted as the condition evolves over time.
Topical Treatments
Topical therapy forms the foundation of eczema management for most patients. Medicated anti-inflammatory creams are used to control active inflammation during flare-ups. These treatments help reduce redness, itching, and skin thickening when used appropriately and for the correct duration.
Non-steroidal topical treatments may be prescribed for sensitive areas such as the face, eyelids, neck, and skin folds, or for long-term maintenance therapy to reduce flare frequency.
Barrier repair therapy is a key component of eczema care. Regular use of appropriate moisturisers helps restore the skin's protective function, reduce water loss, and improve treatment response.
Your dermatologist will guide you on correct application technique, appropriate treatment strength, and clear treatment plans in order to ensure optimal effectiveness and safety.
Systemic Treatments for Moderate to Severe Eczema
For patients with moderate to severe eczema that does not respond adequately to topical treatment alone, systemic therapy may be considered.
Oral medications may be prescribed to reduce inflammation and immune overactivity. These treatments are typically used for more extensive or treatment-resistant eczema and require careful monitoring.
Biologic therapies are advanced treatments that target specific immune pathways involved in eczema. They may be appropriate for selected patients with severe or persistent disease and are prescribed under specialist supervision.
Phototherapy
Phototherapy uses controlled medical-grade ultraviolet light to reduce skin inflammation and itch. It may be recommended for patients with widespread eczema or chronic disease that has not responded sufficiently to topical treatment.
Phototherapy is administered in a clinical setting under dermatological supervision to ensure safety and effectiveness. Treatment schedules and duration will be customised depending on one's individual response.
Tips on Daily Eczema Care and Flare Prevention
Consistent daily care is key for long-term eczema control. Good skincare habits help restore the skin barrier, reduce irritation, and prevent frequent flare-ups.
Gentle Cleansing and Bathing
Regular Moisturising
Early Management of Flares
Trigger Identification and Avoidance
Clothing and Environmental Care
Itch Control and Skin Protection




When Should You See a Dermatologist for Eczema?
You should consider seeing a dermatologist if eczema symptoms persist despite over-the-counter treatments, flare-ups are frequent or severe, itching affects sleep or daily life, signs of skin infection develop, or the diagnosis is uncertain.
Specialist care is particularly important for children, adults with chronic hand eczema, or patients requiring advanced therapies.
FAQs About Eczema
No. Eczema is not contagious and cannot be spread through physical contact, sharing personal items, or close interaction with others.
Eczema is a chronic condition and cannot be permanently cured. However, with appropriate treatment and daily skincare, many patients achieve long periods of good control or remission.
When used correctly under medical guidance, medicated creams are safe and effective for controlling inflammation. Problems usually arise from incorrect strength, prolonged unsupervised use, or improper application.
Diet may play a role in selected individuals, particularly in children, but it is not the primary cause of eczema. Dietary changes should be medically assessed to avoid unnecessary or harmful food restrictions.
Some children experience improvement of eczema as they grow older. Others may continue to have symptoms into adolescence or adulthood, especially if eczema is more severe or persistent.
Yes. Scratching and skin barrier damage can increase the risk of bacterial or viral skin infections. Early treatment is very important if signs of infection develop.
Seek Proper Dermatologist Care for Eczema
If you or your child are experiencing persistent or worsening eczema, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in eczema treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh