Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
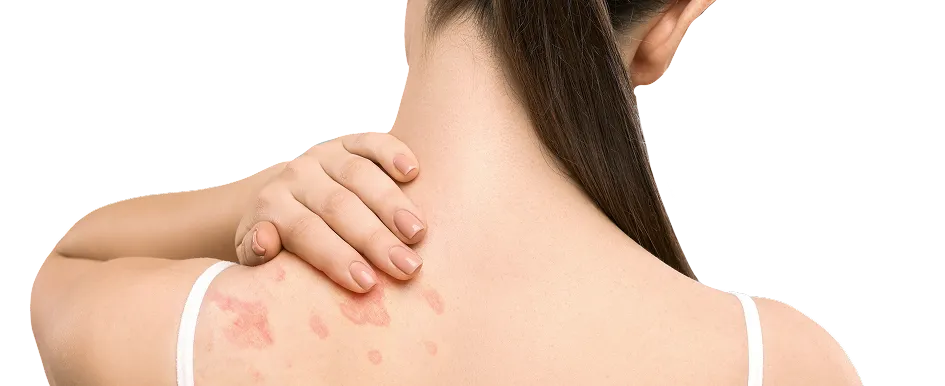
Hives, or urticaria, is a common skin reaction characterized by the sudden appearance of intensely itchy, red, and swollen welts on the skin. These welts, known as wheals, can vary in size and shape, often appearing and disappearing within hours. While most cases are acute and resolve quickly, some individuals suffer from chronic hives that persist for weeks or months, significantly impacting daily comfort, sleep, and overall quality of life.
With proper diagnosis, identification of potential triggers, and personalised treatment under the guidance of a dermatologist, hives can be managed effectively to improve one's comfort and appearance.



What Are Hives?
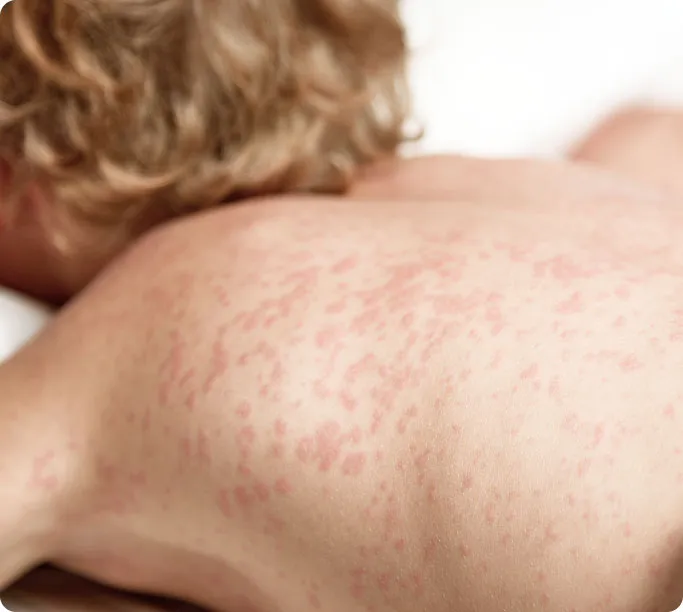
Hives occur when your immune system reacts to a trigger by releasing histamine and other chemicals into the skin. This causes the small blood vessels under the skin to leak fluid, resulting in localized swelling, redness, and itching. Sometimes, they may cause swelling around the eyes or on the lips, known as angioedema.
Hives are not simply an allergic reaction to food. Instead, they can be triggered by a wide range of factors, including infections, stress, pressure, or physical stimuli. Because symptoms can range from mild itching to severe swelling of deeper tissues, professional dermatological care is often required to identify the root cause and provide effective relief.
What Are Common Types of Hives?
Urticaria, or hives, is categorized primarily by the duration of the symptoms and the specific nature of the triggers. Understanding these classifications is key to selecting the right treatment approach.
Acute Urticaria
Chronic Urticaria
Dermographism
Recurrent Keloids
Cholinergic Urticaria
Triggered by a rise in core body temperature, leading to an inflammatory response.
- Occurs during exercise, hot showers, or periods of high emotional stress and sweating.
- Typically manifests as very small, intensely itchy wheals surrounded by large red flares.
Pressure Urticaria
- Develops in response to sustained pressure on the skin, such as from tight waistbands, bra straps, or standing for long periods.
- Unlike other hives, these may not appear until several hours after the pressure was applied and can feel more painful or burning than itchy.
Common Symptoms of Hives to Look Out For
Hives (urticaria) can vary greatly in appearance and sensation depending on the underlying trigger and the severity of the immune response. Below are some common symptoms to look out for.
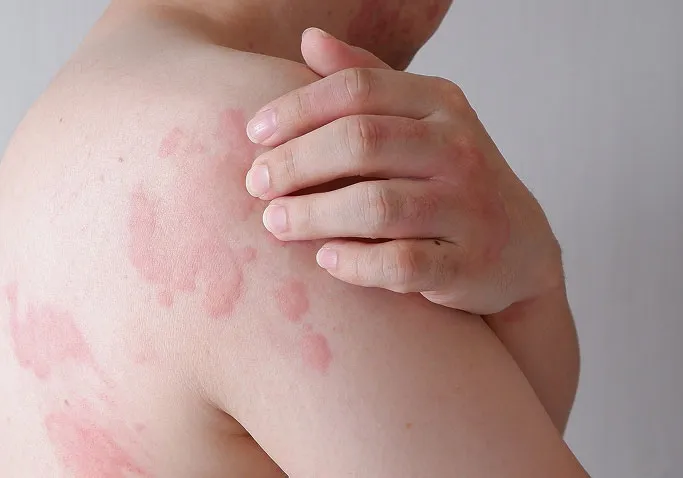
Raised Red or Skin-Coloured Wheals
The most recognizable sign of hives is the sudden appearance of raised bumps or patches on the skin, known as wheals. These can range in size from small pinpoints to large plates several centimeters in diameter.
Intense and Persistent Itching
Nearly all cases of hives are accompanied by an intense itch that can be relentless. This itching often worsens at night or when the skin is warm (such as after a shower or during exercise).
Migrating Rash
A unique characteristic of hives is their fleeting nature. Individual wheals typically disappear within 24 hours, only for new ones to emerge in a different location. This gives the appearance of a rash that travels across the limbs, trunk, or face.
Angioedema/Deep Tissue Swelling
In some people with hives, the reaction also involves deeper layers of the skin. It commonly affects the eyelids, lips, tongue, or genitalia. Angioedema may feel more like a dull ache, burning sensation, or localized numbness.
Stinging or Burning Sensations
While itching is the primary symptom, some patients describe a painful stinging or burning sensation. This can make the skin feel extremely sensitive to the touch or to the friction of tight clothing.
Skin Writing (Dermatographism)
In certain types of physical hives, simply scratching or rubbing the skin can trigger a localized flare-up. This often appears as linear, raised red welts that trace the exact path of the scratch.
Changes in Colour and Texture
When hives are inflamed, the skin may appear bright red or purple. As the wheals resolve, they typically leave no permanent mark, though in individuals with darker skin tones, temporary post-inflammatory hyperpigmentation may occur.
Systemic Symptoms
In severe allergic episodes, hives may be accompanied by systemic signs such as lightheadedness, a racing heart, or gastrointestinal upset. If hives are accompanied by difficulty breathing, wheezing, or a feeling of the throat closing, it is a medical emergency (anaphylaxis) and requires immediate care.
What Causes or Triggers Hives?
Hives occur when specific cells in the immune system, called mast cells, release histamine and other inflammatory chemicals into the bloodstream. This causes small blood vessels to leak fluid, resulting in the characteristic swelling and itching of the skin. While the exact cause is not always identifiable, the following are some known contributors and triggers.
Allergic Reactions
One of the most common causes of acute hives is an allergic response to substances entering the body.
-
Foods
Common culprits include shellfish, nuts, eggs, milk, and certain fruits. -
Medications
Reactions to antibiotics (like penicillin), NSAIDs (like aspirin or ibuprofen), or ACE inhibitors used for blood pressure.
Physical Stimuli
For some individuals, the skin reacts directly to physical environmental changes.
-
Temperature
Exposure to extreme cold (ice, cold water) or high heat (hot showers, sun exposure). -
Pressure and Friction
Tight clothing, heavy bags, or even the act of scratching the skin (dermographism). -
Exercise
Increased core body temperature and sweating (cholinergic urticaria) during physical activity.
Autoimmune and Internal Factors
In chronic urticaria (lasting over 6 weeks), the immune system may mistakenly attack the body's own tissues.
-
Antibodies
The body may produce autoantibodies that continuously activate mast cells. -
Associated Conditions
Hives can sometimes be associated with thyroid disease, lupus, or other systemic inflammatory disorders.
Infections
In many cases, hives are a systemic response to an underlying infection rather than a direct allergy.
-
Viral Infections
Common colds, influenza, or glandular fever are frequent triggers, particularly in children. -
Bacterial/Parasitic
Chronic hives can sometimes be linked to sinus infections, urinary tract infections, or even H. pylori in the stomach.
Environmental Allergens and Stings
Direct contact with or inhalation of certain substances can trigger a localized or widespread flare.
-
Insect Venom
Stings from bees, wasps, or fire ants. -
Contact Allergens
Touching latex, certain chemicals, or pet dander. -
Airborne Particles
Pollen and mold spores can occasionally manifest as skin symptoms.
Emotional Stress
Hormonal Changes
How Are Hives Diagnosed?
Hives are typically diagnosed through clinical evaluation of the rash together with a review of symptoms, medical history, and potential triggers. Additional tests may be performed when an underlying cause is suspected.
Clinical Examination
Medical and Symptom History
Trigger Assessment
Blood Tests (If Needed)
Allergy Testing (Selected Cases)
How Are Hives Treated at TSN Dermatology?
Effective management of hives requires a comprehensive and personalised strategy that focuses on symptom relief, identification of triggers, and long-term stabilization of the immune system.
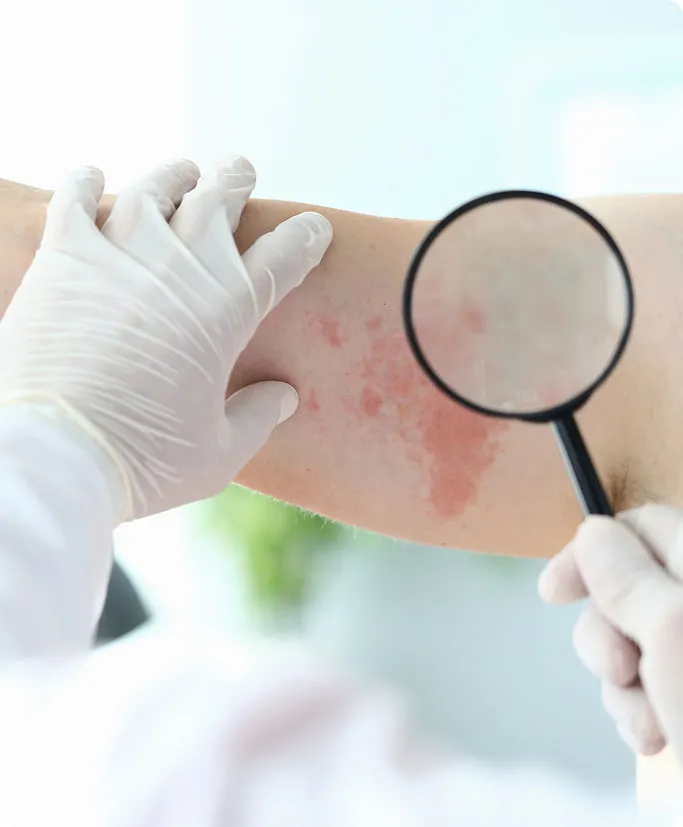
Individualised Treatment
As hives present differently in every patient—ranging from mild, occasional itching to severe, daily wheals—treatment is never one-size-fits-all. Our approach is based on:
Trigger Analysis
A thorough review of potential allergens, medications, infections, or physical stimuli (like heat or pressure) that may be inducing the flare-ups.
Severity Assessment
Evaluating the extent of skin involvement and whether symptoms include angioedema (deep swelling) or systemic signs.
Impact on Quality of Life
Considering how the itch and rash affect your sleep, concentration, and daily activities.
Step-Up Therapy
Gradually adjusting treatment intensity to gain full control over mast cell activity and prevent the return of wheals.
Antihistamine Therapy
Many cases of urticaria can be satisfactorily treated with antihistamines. These medications work by blocking the effects of histamine, the primary chemical responsible for the redness, swelling, and itching of hives.
Dosage Guidance
The dose required to control hives may be higher than the standard dose typically obtained over the counter. Our specialists will guide you on how to safely adjust your dosage to gain complete control.
Non-Drowsy Formulations
We prioritize modern, second-generation antihistamines that provide effective relief without the sedative side effects of older medications.
Advanced Treatments for Severe or Persistent Hives
When hives remain uncontrolled despite standard antihistamine therapy, advanced treatments may be recommended. These therapies target the underlying inflammatory and immune mechanisms responsible for persistent urticaria.
Short Courses of Steroids
Used primarily for acute, severe flares to rapidly calm intense inflammation and provide immediate relief.
Cyclosporine
An immunosuppressant that can be highly effective for refractory chronic urticaria by suppressing the overactive immune response.
Biologic Therapy (Omalizumab/Xolair)
For patients with chronic spontaneous urticaria who do not respond to antihistamines, this targeted injectable therapy offers a high degree of efficacy and safety, often leading to complete remission.
Avoidance and Environmental Control
Managing hives also involves identifying and minimising exposure to known triggers. Once potential triggers are recognised, practical avoidance strategies and lifestyle adjustments can help reduce the frequency and severity of flare-ups and improve long-term symptom control.
Allergen Avoidance
Clear protocols on avoiding specific food or medication triggers once they have been identified.
Physical Stimuli Management
Practical strategies for patients with physical urticaria, such as cooling techniques for heat-induced hives or avoiding mechanical pressure on the skin.
Emergency Preparedness
For patients at risk of severe reactions, we provide training on the use of emergency medications and the development of a comprehensive safety plan.
Tips on Daily Care and Prevention for Hives
For individuals prone to urticaria, daily care focuses on avoiding triggers and reducing skin irritation. Simple lifestyle and skincare measures can help minimise flare-ups and the severity of symptoms.
Trigger Identification and Environmental Control
-
Maintain a Trigger Diary
Track activities, diet, medications, and stress levels alongside flare-ups to help identify possible triggers. -
Manage Ingested Triggers
If certain foods or medications trigger your hives, check ingredient labels carefully and inform your doctor or pharmacist about your allergies so they can avoid prescribing medications that may cause a reaction.
Gentle Skin Care and Hygiene
-
Use Lukewarm Water
Avoid hot showers or baths, which may worsen itching and swelling. -
Fragrance-Free Cleansing
Use gentle, soap-free and fragrance-free cleansers to reduce skin irritation. -
Moisturise Regularly
Apply bland moisturisers to maintain the skin barrier and soothe itchy areas.
Environmental and Lifestyle Factors
-
Stay Cool
Heat and sweating can trigger hives in some individuals. Keep cool and shower after heavy sweating. -
Stress Management
Emotional stress may worsen symptoms. Relaxation techniques such as deep breathing or meditation may help.
Itch Control and Physical Protection
-
Avoid Scratching
Scratching can worsen inflammation and trigger more hives. Cold compresses or anti-itch lotions may help relieve discomfort. -
Wear Loose Clothing
Choose loose, breathable fabrics to reduce friction and pressure on the skin. -
Keep Fingernails Short
Short nails reduce the risk of skin damage and infection if scratching occurs.
Medication Adherence and Preparedness
-
Take Antihistamines as Advised
Proper use of prescribed antihistamines can help prevent flare-ups. -
Carry Emergency Medication
Patients with severe reactions or angioedema should keep emergency medication readily available.



When Should You See a Dermatologist for Hives?
While a single, mild episode of hives can usually be managed on one's own, proper medical intervention is advised when symptoms are so severe or persistent that they disrupt your quality of life. See a dermatologist if you experience any of the following:
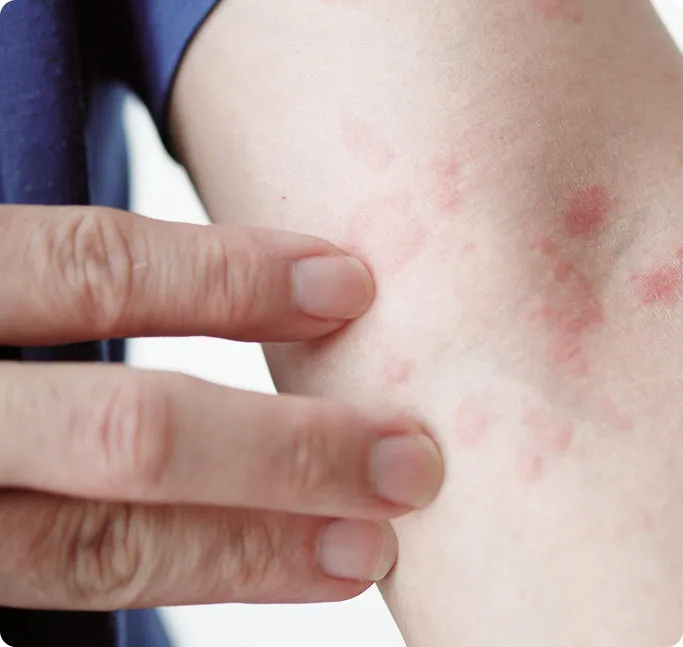
Persistent or Chronic Symptoms
If your hives occur nearly every day for more than six weeks, you may have chronic spontaneous urticaria. Unlike short-term hives, this condition is usually not caused by a clear trigger. A specialist may evaluate possible underlying causes and recommend treatments to manage the condition.
Presence of Angioedema (Deep Swelling)
If your hives are accompanied by significant swelling of the eyelids, lips, tongue, or hands, this means that the inflammatory response is affecting deeper layers of the skin. If you experience any swelling in the throat or difficulty breathing, seek medical attention immediately.
Inadequate Relief from OTC Treatments
If you have been using over-the-counter antihistamines for several weeks without a meaningful reduction in the itching or the number of wheals, you may require prescription-strength therapies, such as higher-dose H1-antagonists or targeted biologics.
Painful or Bruising Welts
Standard hives are itchy and resolve without leaving a mark. If your welts are painful, tender to the touch, or leave behind a bruise-like stain (purpura) after they fade, this could be a sign of urticarial vasculitis (inflammation of the blood vessels), which requires further medical evaluation.
Physical Triggers (e.g Heat, Cold, or Exercise)
If your hives are repeatedly triggered by physical factors, a dermatologist can help identify the specific trigger and recommend strategies to manage symptoms and prevent flare-ups.
Impact on Mental Well-being and Sleep
Chronic itching is physically and mentally draining. If your hives are causing major sleep disturbances, anxiety, or social withdrawal due to the appearance of the rash, a specialist can provide more effective treatments and the peace of mind you deserve.
FAQs About Hives
No. Hives are not contagious and cannot be spread through physical contact, sharing personal items, or close interaction with others. They occur when the skin's immune system reacts to certain triggers, such as allergies, infections, medications, or stress.
Acute hives typically resolve once the trigger is removed. Chronic hives are more challenging but are manageable. Tailored, long-term treatment with antihistamines or biologics can usually lead to long periods of remission where the skin remains clear.
Yes, when used according to a dermatologist's guidance. Many modern antihistamines are designed for long-term safety and typically do not cause the drowsiness or brain fog associated with older medications; and can be effective at managing chronic hives.
Hives occur because your immune system has a unique threshold for certain triggers. This can be due to genetic predisposition, your current immune status, or recent illnesses. In chronic cases, your mast cells may be hyper-reactive, releasing histamine in response to stimuli that others' bodies would simply ignore.
While food allergies are a common cause of acute hives, they are rarely the primary cause of chronic hives (urticaria lasting over 6 weeks). In chronic cases, the triggers are usually internal immune signals. It is important to be medically assessed before starting a restrictive diet to ensure you aren't avoiding foods unnecessarily.
Seek Proper Dermatologist Care for Hives
If you or your child are experiencing Hives, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in hives treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh