Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
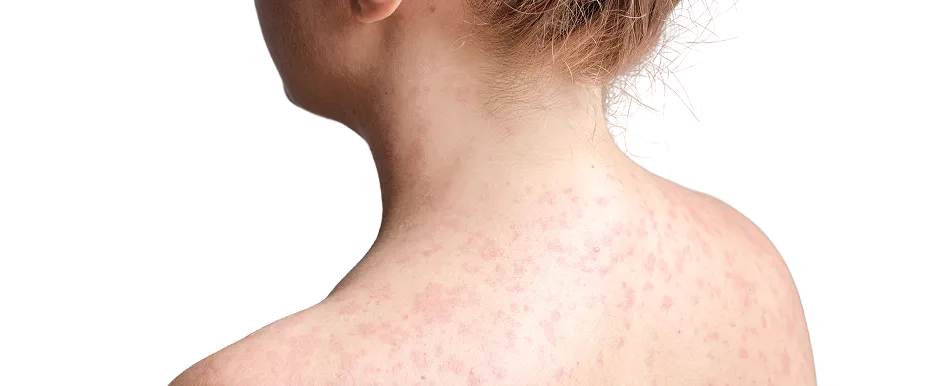
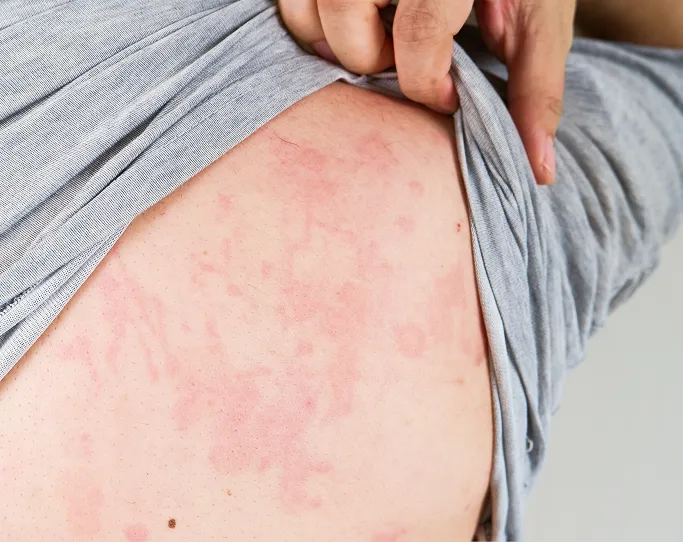
Allergies are immune system responses to substances that are typically harmless, such as pollens, fragrances, metals, or medications. When a person with a skin allergy encounters their specific trigger, their immune system overreacts, producing immune responses that release inflammatory chemicals such as histamine or activate other immune pathways. This reaction often manifests on the skin, ranging from mild itching to severe, painful rashes that can significantly impact daily activities and physical well-being.
While there is often no immediate cure that eliminates an allergy entirely, most patients can achieve significant relief and skin clearance through accurate diagnosis, strategic avoidance, and personalised management plans guided by a dermatologist.



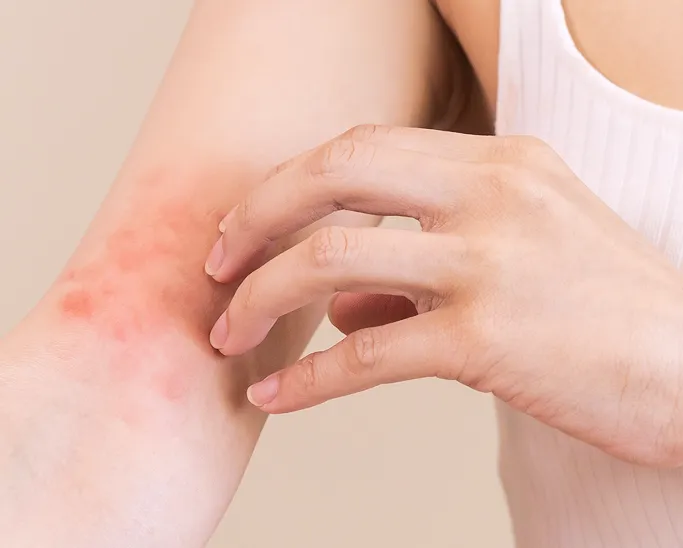
What is a Skin Allergy?
A skin allergy occurs when your immune system misidentifies a harmless substance, such as a cosmetic preservative, a metal in your jewellery, or a specific medication, as a dangerous invader. In response, your body activates an immune response. In some cases, this involves antibodies such as Immunoglobulin E (IgE), while in others, it involves delayed immune reactions mediated by specialised immune cells.
It is a complex immune-mediated condition that frequently presents as a localised reaction on the skin barrier. Because reactions can range from simple redness and itching to severe blistering or systemic swelling, a professional evaluation by a dermatologist is essential for accurately identifying your triggers and developing an effective management and safety plan.
What are Common Types of Skin Allergies?
While allergies can affect multiple organ systems, dermatologists primarily focus on reactions that manifest on the skin barrier. Accurate diagnosis of the specific category is essential for effective symptom control and long-term safety.
Hives (Urticaria)
- Can be triggered by factors such as medications, infections, foods, or physical stimuli. In many chronic cases, no specific external allergen is identified.
- Characterised by sudden, raised, red, and itchy welts that can appear anywhere on the body and may shift locations within hours.
Allergic Contact Dermatitis
- Occurs when the skin directly touches an allergen, such as nickel (often found in jewellery, watch straps, or belt buckles), fragrances, preservatives in skincare, hair dyes, or latex.
- Typically appears as a red, intensely itchy, or blistering rash localised specifically to the area of contact.
Eczema/Rashes
- A chronic condition where the skin barrier is compromised, making it more sensitive to environmental triggers such as irritants, climate changes, and, in some individuals, allergens like dust mites or pet dander.
- Presents as dry, red, and scaly skin, often accompanied by persistent itching that can fluctuate depending on environmental and internal factors.
Insect Sting Allergies
- While local swelling is common, some individuals develop a systemic allergic skin response to the venom from stinging insects like bees, wasps, or hornets.
- Requires careful monitoring, as systemic reactions can progress rapidly beyond the skin and become life-threatening.
Oral Allergy Syndrome (OAS)
- A cross-reaction between airborne pollen allergies and certain raw fruits, vegetables, or nuts.
- While primarily causing oral symptoms (itching or swelling of the lips, tongue, and throat), it may occasionally be associated with mild irritation around the mouth.
Drug-Induced Eruptions
- An immune-mediated reaction to medications, most commonly antibiotics, anti-inflammatory drugs, or anticonvulsants.
- Can manifest as widespread skin rashes, hives, or in rarer, more severe cases (such as Drug Reaction with Eosinophilia and Systemic Symptoms or SJS/TEN), widespread blistering and peeling.
Common Symptoms of Skin Allergies to Look Out for
As skin allergies can manifest in a wide variety of ways, recognising the early signs is critical for seeking timely professional advice. While some reactions are immediate, others may be delayed by hours or even days. If you notice any of the following, we recommend scheduling an evaluation at our clinic:
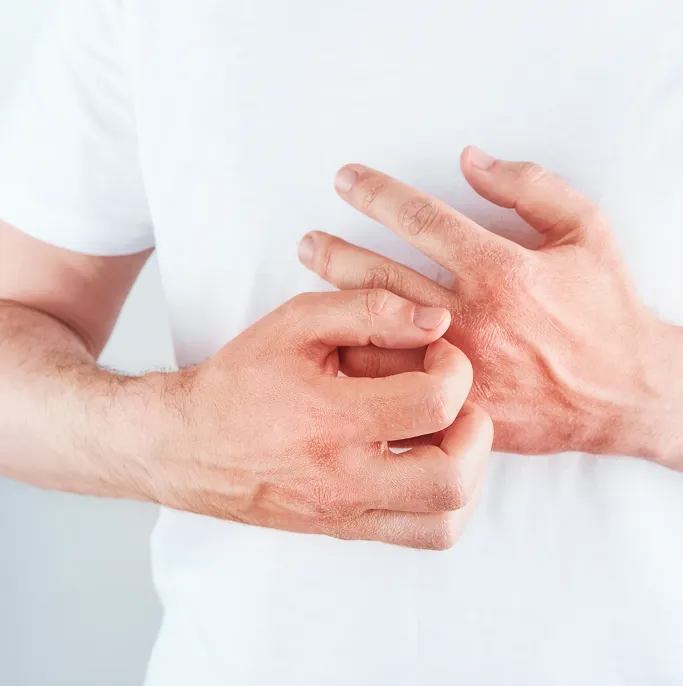
Persistent or Intense Itching
Redness and Inflammation
Skin Rashes and Hives
Dryness, Scaling, and Flaking
Blisters and Weeping
Swelling
Burning or Stinging Sensation
What Causes or Triggers an Allergic Reaction?
An allergic reaction occurs when your immune system encounters a substance, known as an allergen, that it incorrectly identifies as a harmful invader. For individuals with allergies, even trace amounts of these common substances can provoke a protective, yet overzealous, immune response. In our tropical climate in Singapore, these triggers can come from your environment, your personal care products, or even your diet.
Inhaled Environmental Allergens
These are airborne substances that enter the respiratory system and trigger skin conditions like eczema or skin irritation.
-
Pollen
Tiny particles from trees, grasses, and weeds that are present year-round, though levels may fluctuate. -
Dust Mites
Microscopic organisms thriving in carpets, bedding, and upholstery. -
Pet Dander
Tiny flecks of skin shed by cats, dogs, and other animals. -
Mould
Fungal spores that flourish in damp, poorly ventilated indoor or outdoor environments.
Medications and Treatments
-
Topical Medications
Ironically, substances meant to treat skin issues, such as antibiotic ointments or certain topical steroids, can sometimes trigger an allergic reaction in sensitive individuals. -
Systemic Medications
Oral antibiotics, anti-inflammatory drugs, and anticonvulsants are common culprits for drug-induced skin eruptions or hives.
Direct Contact Irritants and Allergens
-
Personal Care Products
Fragrances, preservatives, and specific chemical compounds found in soaps, shampoos, lotions, and deodorants are frequent causes of allergic contact dermatitis. -
Metals
Nickel, cobalt, and chromium are common triggers found in everyday items such as jewellery, watches, belt buckles, and even keys. -
Materials
Latex (found in gloves, balloons, or medical supplies) and certain dyes used in clothing can trigger localised skin reactions upon contact.
Dietary Triggers
-
Food Proteins
Common food allergens include peanuts, tree nuts, shellfish, eggs, milk, soy, and wheat. While often associated with gastrointestinal or respiratory symptoms, these may, in some individuals, manifest as acute hives or skin rashes. -
Oral Allergy Syndrome (OAS)
This occurs when the proteins in certain raw fruits or vegetables closely resemble the pollen you are allergic to, causing itching or swelling specifically around the mouth and lips upon consumption.
How are Allergies Diagnosed?
Accurate diagnosis is crucial, as many conditions, such as skin irritations, can mimic allergic reactions and require different management approaches. A dermatologist may assess your condition using the following methods:
Diagnostic Testing
Once we narrow down the potential culprits, we may use one or more of the following tests to confirm the diagnosis:
-
Patch Test
This is the gold standard for identifying allergic contact dermatitis. We apply patches containing common suspected allergens (such as hair dye, nickel, preservatives, and fragrances) to your back under adhesive tape. These remain in place for 48 to 72 hours. Upon removal, our dermatologists examine the area to identify any abnormal skin reactions. -
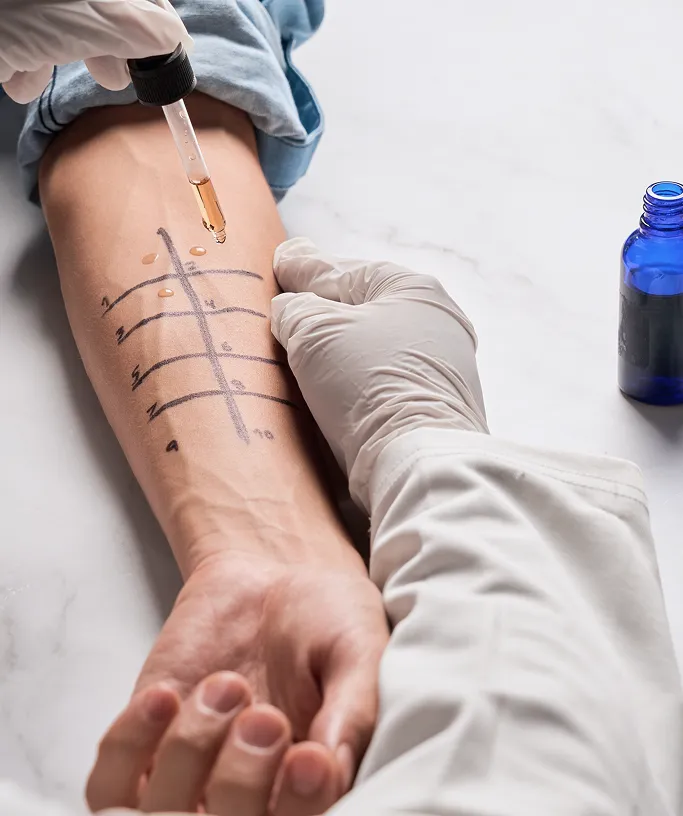
Prick Test
This test is used to evaluate immediate-type allergies to foods and airborne substances. Testing for medication allergies is more specialised and only available for selected drugs. A small drop of the suspected allergen is placed on the skin and introduced via a tiny, gentle prick. This process is generally not painful, is suitable for both adults and children, and provides results in about 20 minutes. -
Blood Test (Specific IgE)
When a person is suspected of having a systemic allergy to foods, medications, or airborne substances, we may perform a blood test. This measures the levels of IgE (an antibody produced by your immune system) in your blood, providing supportive information about your immune response to specific triggers when interpreted alongside your clinical history.
Clinical Examination and Medical History Review
We begin with a comprehensive review of your medical history, recent exposures, and lifestyle habits. We will discuss:
-
The Pattern of Reaction
When and where the reaction occurs, and how long it lasts. -
Environmental & Product Exposure
Any new skincare, makeup, jewellery, or household products you have introduced recently. -
Potential Triggers
Your history with specific foods, medications, or airborne substances.
Interpreting Your Results
How are Skin Allergies Treated at TSN Dermatology?
Effective allergy management at TSN Dermatology is a two-pronged approach: providing immediate relief from uncomfortable symptoms and developing a long-term strategy to prevent future flare-ups. Because every patient's immune profile is unique, we tailor our treatment plans to your specific triggers, the severity of your reaction, and your lifestyle.
Individualised Treatment Approach
As skin allergies manifest in diverse ways, from the dry, scaly patches of eczema to the painful, blistering rash of contact dermatitis, treatment must be highly customised:
Identification of Triggers
We use clinical history and diagnostic testing (such as patch or prick tests) to pinpoint exactly what your skin is reacting to.
Symptom Profile
We assess whether your reaction is localised to a specific area (like contact with jewellery) or widespread (like medication-induced hives).
Impact on Quality of Life
We address how often your itching, burning, or visible rash interferes with your sleep, work, or physical activities.
Long-Term Safety
For individuals at risk of severe systemic responses (such as drug-induced eruptions), we provide comprehensive safety education and action plans.
Avoidance and Environmental Control
Medications are used to soothe the skin and block the inflammatory chemicals released during a reaction:
Topical Anti-inflammatories
Medicated creams and ointments, such as corticosteroids or calcineurin inhibitors, are our primary tools for calming redness, reducing swelling, and healing the skin barrier.Oral Antihistamines
Particularly useful for controlling itching and hives in conditions such as urticaria.Barrier Repair Creams
We prescribe specialised emollients to repair the skin's natural defences, which help protect you from future environmental irritants.
Advanced and Targeted Therapies
For patients who struggle with chronic, persistent skin allergies that do not respond to standard care, we offer advanced treatment options:
Biologic and Immunomodulatory Treatments
For severe conditions like chronic atopic dermatitis (eczema), we offer targeted therapies that work systemically to calm an overactive immune response.Phototherapy
In some cases, we use controlled exposure to medical-grade light to modulate the skin's immune response and reduce chronic inflammation.Allergen Avoidance Strategies
Once a contact allergen is identified, we provide detailed guidance on how to avoid it in daily life, including product selection and environmental modifications.
Tips on Daily Care and Prevention for Skin Allergy
Managing skin allergies requires a proactive approach to protecting your skin barrier and minimising exposure to triggers that cause your immune system to flare. By integrating these habits into your daily routine, you can soothe active inflammation and significantly reduce the frequency of future skin reactions.
Environmental & Contact Control
-
Fragrance-Free Living
Fragrances in soaps, detergents, and body washes are common triggers for allergic contact dermatitis. Switch to fragrance-free, hypoallergenic, and soap-free cleansers to minimise irritation. -
Textile Choices
Wear loose-fitting, breathable natural fibres like cotton. Avoid rough wool or synthetic fabrics that can trap sweat and friction, which often exacerbate allergic rashes like eczema. -
Nickel Awareness
If you have a known nickel allergy, ensure your watch straps, belt buckles, and jewellery are nickel-free or coated. Consider using clear nail polish on the back of metal buttons to create a barrier between the metal and your skin. -
Control Indoor Humidity
While Singapore's humidity is high, keep your bedroom environment stable. Excessive moisture in the air can encourage mould and dust mite growth, which can worsen skin symptoms for patients with atopic dermatitis.
Personal Care and Hygiene
-
Gentle Cleansing
Shower in lukewarm water, not hot, to prevent stripping the skin of natural oils. Apply a fragrance-free, hypoallergenic moisturiser within 3 minutes of showering to lock in hydration and reinforce your skin's protective barrier. -
Post-Exposure Care
If you have been outdoors or in a dusty environment, pollen and pollutants can settle on your skin and trigger a reaction. Rinse off gently to remove these environmental allergens as soon as you return home.
Preparedness and Medical Management
-
Follow Your Treatment Plan
If prescribed topical steroids or immunomodulators, use them exactly as directed. These medications are designed to reduce inflammation at the cellular level; stopping them too soon can cause the rash to rebound quickly. -
Carry Your Emergency Plan
If you are prone to severe systemic skin reactions (like hives or angioedema), always carry your prescribed antihistamines and, if directed, your emergency medication. -
Know Your Limits
If you notice a rash is spreading, weeping, or becoming painful, do not wait for it to clear on its own. Contact our office for an early evaluation to prevent secondary infections or scarring.
Lifestyle and Monitoring
-
Symptom & Exposure Diary
Keep a log of your flares. Note any new products (cosmetics, hair dyes, household cleaners), foods, or environments you were exposed to in the 48 hours before a rash appeared. This record is invaluable for your dermatologist during your next visit. -
Read Ingredient Labels
Develop the habit of scanning the ingredient lists on your shampoos, lotions, and cosmetics for known allergens (such as preservatives like methylisothiazolinone or common fragrances) that your doctor has identified as your personal triggers. -
Sun Protection
Use mineral-based sunscreens (containing zinc oxide or titanium dioxide) rather than chemical sunscreens, which are more likely to cause allergic reactions in sensitive skin.



When Should You See a Dermatologist for Skin Allergies?
While mild, one-time reactions to a new soap or piece of jewellery can sometimes be managed at home, persistent or severe skin allergies require professional evaluation. Skin conditions can be deceptively similar, and a dermatologist's expertise is necessary to distinguish between a simple irritation, an allergic reaction, and other chronic conditions like psoriasis or autoimmune disorders.You should schedule an appointment at TSN Dermatology if you experience any of the following:

Persistent or Recurring Rashes
If a rash lasts longer than two weeks, or if it frequently clears up only to return in the same spot, you likely have an unidentified contact allergen that needs to be pinpointed.
Signs of Secondary Infection
If your skin becomes warm, develops pus, yellow crusting, or painful, spreading redness, the skin barrier may be infected and requires professional treatment to prevent scarring.
Symptoms Impacting Daily Life
If itching is so intense that it prevents you from sleeping, concentrating at work/school, or engaging in normal physical activities, it is time for medical intervention.
Widespread Reactions
Any rash that covers a large surface area of your body, especially if it is accompanied by systemic symptoms like fever, chills, or swelling of the eyelids or lips, warrants an urgent evaluation.
Failure of Over-the-Counter Remedies
If you have tried standard antihistamines or over-the-counter moisturisers for more than a week without significant improvement, you likely need a stronger, prescription-grade treatment.
Uncertainty of Diagnosis
If you are unsure whether your bump or rash is an allergy, an insect bite, an infection, or a precancerous lesion, avoid the wait-and-see approach. We can provide an accurate diagnosis, which is the foundation of any effective treatment plan.
FAQs About Skin Allergies
Allergies can be effectively managed, but not fully cured. By identifying your specific triggers through patch or prick testing, using targeted anti-inflammatory treatments to restore the skin barrier, and learning strategic avoidance, most patients can achieve clear, comfortable skin, achieve good symptom control and long-term skin stability.
While many skin allergies like eczema often start in childhood, adults can develop new sensitivities at any age. Changes in your immune system, long-term exposure to certain chemicals (like those found in skincare or work environments), or even hormonal shifts can cause your skin to suddenly react to substances that previously caused no issues.
In Singapore's tropical climate, skin allergies often flare due to a combination of factors. Higher humidity can promote mould growth and dust mites, while increased sweating can trap allergens against your skin, leading to more frequent contact dermatitis or prickly sensations. Additionally, seasonal shifts in airborne pollutants can exacerbate underlying conditions like atopic dermatitis.
Contact allergies (like an allergy to nickel, fragrances, or preservatives) generally do not disappear on their own. Once your immune system has developed a memory for a specific contact allergen, it will likely continue to react to it upon exposure. The most effective strategy is consistent avoidance and using barrier-protecting products to minimise reaction risk.
Yes. This is a common phenomenon called sensitisation. Your immune system can become sensitised to an ingredient (such as a preservative in your favourite moisturiser) after years of use. If you suddenly develop redness, itching, or peeling after using a familiar product, it may be time for a patch test to identify if one of its ingredients has become a new trigger.
Seek Proper Dermatologist Care for Skin Allergies
If you or your child are experiencing persistent or worsening allergic reactions, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in skin allergy treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh