Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
A skin infection occurs when pathogens—such as bacteria, fungi, or viruses—invade the skin's protective barrier and multiply within the tissue. Infections are dynamic and can progress, spread, or cause systemic symptoms like fever and pain if left untreated. While some minor infections resolve with basic hygiene, many require precise medical diagnosis to prevent complications, scarring, or further transmission to others.
With professional dermatological assessment, the specific pathogen can be identified, and targeted treatments—such as antibiotics, antivirals, or antifungals—can be administered to clear the infection and restore your skin's health.



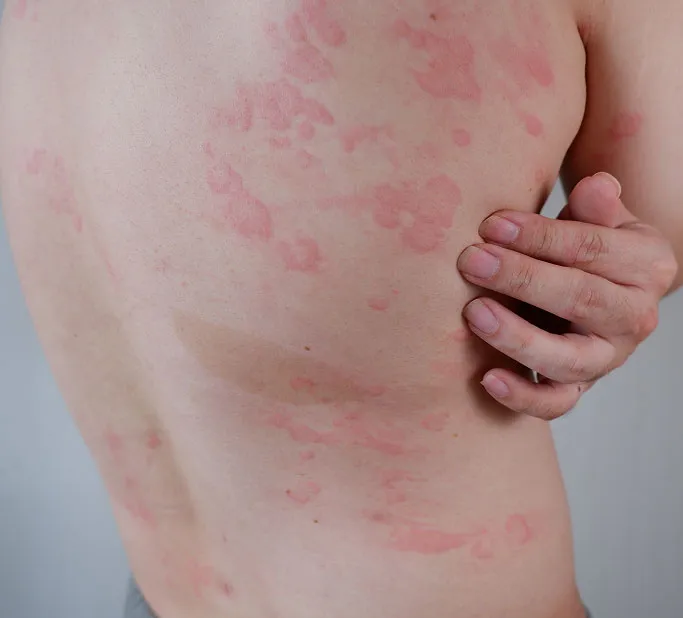
What Is a Skin Infection?
A skin infection is a condition where microorganisms disrupt the integrity of the skin. The cause depends on the type of pathogen involved: bacteria (e.g., staphylococcus), fungi (e.g., ringworm), or viruses (e.g., HPV or shingles). The defining characteristic of an infection is that it is often inflammatory, meaning it can cause redness, swelling, warmth, pain, or the production of pus.
It is a common misconception that all red, itchy, or swollen patches are simply allergies or irritation. Because certain skin infections can mimic inflammatory conditions, specialised dermatological examination is required to differentiate the cause. If a lesion is persistent, spreading, weeping, or accompanied by systemic symptoms such as fever or lethargy, professional evaluation is the only way to ensure an accurate diagnosis and prevent the infection from worsening or spreading to other parts of the body or to other people.
What Are Common Types of Skin Infections?
While many skin infections are mild and self-limiting, they are classified by the specific pathogen—the invader—causing the disruption. Understanding the type of infection you have is essential for determining the correct treatment, as bacterial, viral, and fungal infections each require vastly different therapeutic approaches.
Bacterial Infections
These occur when bacteria, such as Staphylococcus or Streptococcus, enter the skin through small cuts, abrasions, or hair follicles.
-
Abscesses (Boils)
Deep, painful, warm, and red swellings filled with pus. They often occur in hair-bearing areas like the armpits or groin. -
Erysipelas & Cellulitis
These present as painful, spreading red patches that feel warm to the touch. They often cause systemic symptoms like fever and can be particularly dangerous if they affect the legs, making walking difficult.
Fungal Infections
Fungi thrive in warm, moist environments and frequently colonise the skin, nails, or hair.
-
Tinea Infections (Ringworm)
These are identified by their characteristic red, itchy, flaky rings that grow outwards from a centre. Common variants include Tinea cruris (jock itch), Tinea pedis (athlete's foot), and Tinea capitis (scalp infection). -
Pityriasis Versicolour
This yeast-based infection disrupts skin pigment, leading to persistent white, light brown, or red flaky patches. It is particularly common in young adults and often worsens after sweating.
Viral Infections
Viral infections occur when a virus enters skin cells to replicate, often creating distinct surface changes.
-
Viral Warts
Caused by the Human Papillomavirus (HPV), these appear as thickened skin, sometimes with tiny black dots, particularly on the palms and soles. -
Herpes Zoster (Shingles)
A painful, blistering rash that follows a specific nerve distribution (often in a band). It results from the reactivation of the dormant Varicella Zoster virus. -
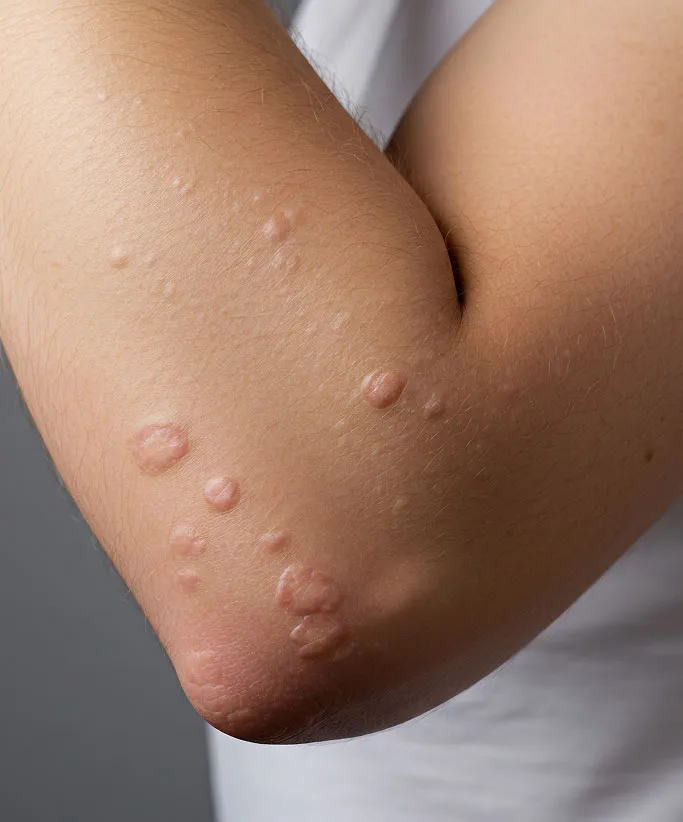
Molluscum Contagiosum
Typically seen in children, this infection presents as smooth, pearly, dome-shaped bumps.
Common Symptoms of Skin Infections to Look Out For
While many skin infections are mild and self-limiting, they can progress rapidly if left untreated. Recognising the early signs of a bacterial, fungal, or viral infection is critical for seeking the correct treatment. Here are the common symptoms to monitor:
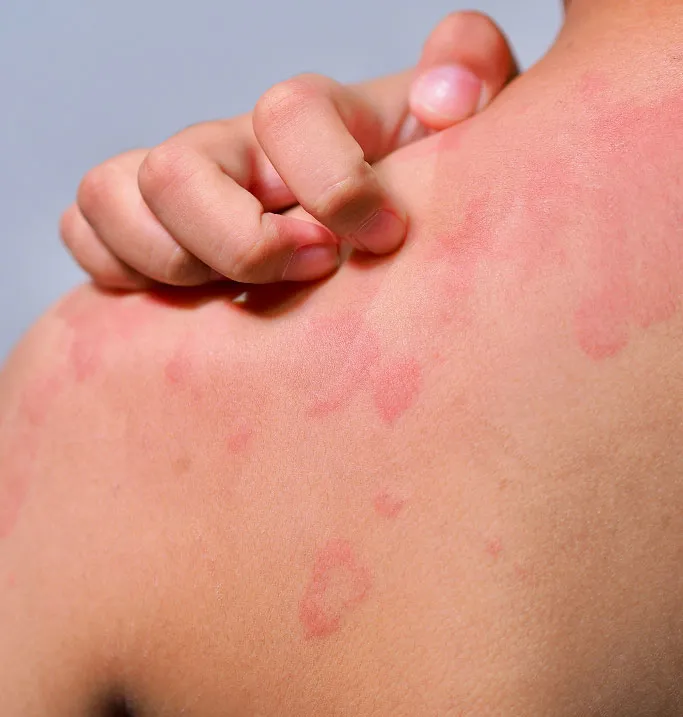
Spreading Redness and Warmth
If you notice a patch of skin that is red, swollen, and feels hot to the touch, it may indicate a bacterial infection like cellulitis or erysipelas. If this redness is rapidly expanding or spreading across your limb, it requires an urgent medical evaluation to prevent the infection from entering the bloodstream.
Presence of Pus or Discharge
The appearance of yellow, cloudy, or malodorous fluid is a hallmark of a bacterial infection, such as an abscess or boil. If you see pus collecting under the skin or weeping from a wound, this indicates that your immune system is actively fighting a bacterial invader and may require professional drainage or antibiotics.
Pain, Tenderness, or Tingling
Most skin infections are accompanied by localised discomfort. A throbbing, painful sensation often points to a deep bacterial abscess, while an unusual tingling or burning sensation occurring before a blistering rash appears is a classic warning sign of Herpes Zoster (Shingles).
Characteristic Rash Morphology
Infections often follow specific, recognisable patterns:
-
Fungal
Look for itchy, flaky rings that grow outward (Ringworm/Tinea) or persistent, discoloured white spots that do not tan. -
Viral
Watch for small, pearly, dome-shaped bumps (Molluscum) or skin thickening with tiny black dots (Warts).
Systemic Symptoms
If a skin infection is accompanied by systemic markers—such as fever, chills, fatigue, or swollen lymph nodes—it suggests that the infection is no longer confined to the surface of the skin. This is a clear indicator that you should seek professional medical intervention immediately.
Persistent or Worsening Condition
While some minor scrapes heal on their own, an infection that remains persistent, increases in size, or fails to respond to basic hygiene and over-the-counter care is a signal to consult a dermatologist. Never attempt to pop or drain a boil yourself, as this can force bacteria deeper into the skin and lead to more serious complications.
What Causes or Triggers Skin Infections?
Skin infections are caused by external pathogens. These organisms invade the skin's protective barrier, multiply, and trigger an inflammatory response.
Bacterial Colonisation
Fungal Overgrowth
Viral Pathogens
Viral infections occur when a virus enters skin cells and hijacks their machinery to replicate.
-
HPV
The Human Papillomavirus causes warts by causing rapid, localised multiplication of skin cells. -
Varicella Zoster
This virus, which causes chickenpox, remains dormant in the nerves for years. When the immune system is stressed or wanes, the virus reactivates, travelling along nerve fibres to the skin to cause shingles.
Impaired Skin Barrier
The skin is the body's primary defence system. When this barrier is disrupted, the body becomes highly susceptible to infection. Common triggers for barrier breakdown include:
-
Chronic Skin Conditions
Eczema or dry skin can cause microscopic cracks that serve as entry points for bacteria. -
Systemic Health
Conditions like diabetes or poor circulation can weaken the immune system and slow the healing process, making it much easier for an infection to take hold and spread.
Close Personal Contact or Fomites
Many infections, particularly viral warts, molluscum, and certain fungal infections, are contagious. They spread through:
-
Direct Contact
Skin-to-skin contact with an infected individual. -
Fomites (Indirect Contact)
Touching contaminated surfaces like shared towels, gym equipment, or floors in public showers.
How Are Skin Infections Diagnosed?
A dermatologist diagnoses a skin infection by evaluating your medical history, clinical symptoms, and the physical appearance of the affected area. Because bacterial, fungal, and viral infections often manifest with similar symptoms—such as redness, scaling, or blistering—a precise clinical assessment is essential to determine the correct pathogen and the most effective treatment.
Clinical Examination and Inspection
Medical History Review
Diagnostic Sampling
If an infection is extensive, recurrent, or resistant to initial treatment, we may need to confirm the diagnosis through laboratory testing:
-
Skin Scrapings (KOH Test)
For suspected fungal infections, a tiny sample of skin cells is scraped and examined under a microscope with potassium hydroxide (KOH) to reveal fungal filaments. -
Swabs and Cultures
If a bacterial infection is suspected (like a persistent boil), we may swab the area to culture the bacteria, identifying the exact strain and determining which antibiotic will be most effective. -
Punch Biopsy
In rare or complex cases where the diagnosis is unclear, a small tissue sample is taken under local anaesthesia to examine the skin architecture under a microscope. This helps us rule out inflammatory conditions that mimic infections.
How Are Skin Infections Treated at TSN Dermatology?
Our treatment approach focuses on safety, precision, and minimising scarring. As infections are caused by living pathogens, our primary goal is to neutralise the invader while simultaneously repairing your skin's damaged barrier to prevent recurrence or scarring.
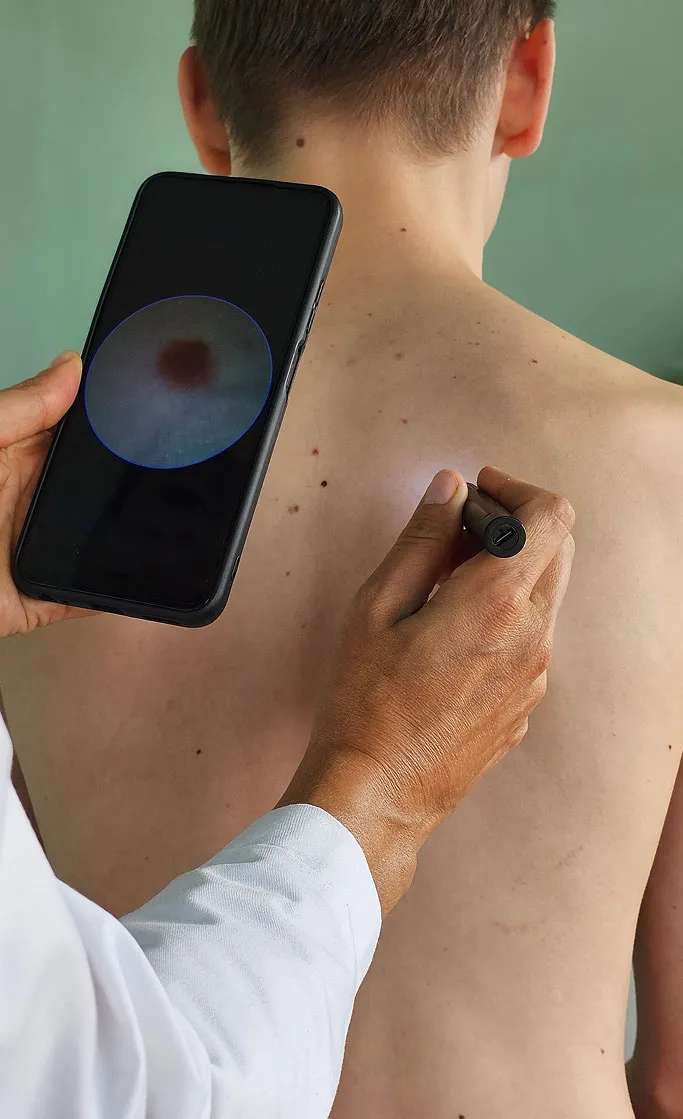
Individualised Treatment Approach
We begin by identifying the specific pathogen. A bacterial boil requires a vastly different approach than a viral rash or a fungal infection. Our treatment plan is determined by the severity of the infection, the depth of tissue involvement, and whether you have underlying health conditions that impact your immune response.
Pharmacological Management
Depending on the diagnosis, we prescribe targeted medications to clear the infection:
Antibiotics
For bacterial infections like cellulitis or abscesses, we use oral or intravenous antibiotics. If you have an abscess, we may perform surgical drainage (incision and drainage) to remove the pus, followed by regular wound dressing to ensure clean healing.
Antifungals
These include specialised topical creams, lotions, or oral tablets designed to disrupt the fungal cell wall. For persistent fungal infections, we may recommend a course of treatment that lasts several weeks to ensure the pathogen is fully eradicated.
Antivirals
For conditions like Shingles (Herpes Zoster), early administration of oral antivirals is critical. These medications work best when started within the first 72 hours, significantly reducing the duration of blistering, the severity of pain, and the risk of long-term nerve-related complications.
Procedural Interventions
For certain viral infections, we offer in-office procedures to expedite recovery:
Cryotherapy: Using liquid nitrogen to freeze and destroy tissue affected by viral warts or molluscum contagiosum.
Extraction: For persistent molluscum, we may perform minor mechanical extraction under topical anaesthesia.
Electrocautery/Laser: These tools can be used to precisely treat viral warts that have proven resistant to topical therapies.
Barrier Repair and Wound Care
Once the infection is cleared, the skin often requires support to recover its structural integrity:
Antiseptic Cleansing: We guide you on the proper use of medical-grade cleansers to keep the affected area free of secondary bacterial colonisation during the healing phase.
Wound Dressing Protocols: For open areas, we provide specific instructions on dressing changes to prevent the wound from drying out or becoming reinfected.
Scar Management: If the infection was deep (as in a severe boil or cellulitis), we may recommend silicone-based treatments to minimise any resulting marks once the infection is fully resolved.
Long-Term Prevention
To ensure you do not experience recurring infections, we work with you to:
Optimise Immune Health: Especially for patients with conditions like diabetes.
Environmental Control: Provide advice on how to manage personal hygiene and shared spaces to prevent the spread of fungal or viral pathogens.
Barrier Protection: Teach you how to properly moisturise and protect skin prone to cracking, which serves as a primary entry point for bacteria.
Tips on Daily Care and Prevention of Skin Infections
Maintaining a healthy skin barrier is your best defence against pathogens. While some infections are unavoidable, these daily habits can significantly reduce your risk of contracting bacterial, fungal, or viral infections and help you manage the skin environment if you are prone to recurring issues.
Maintaining Barrier Integrity
-
Moisturise Daily
A well-hydrated skin barrier is less prone to the microscopic cracks that allow bacteria like Staphylococcus to enter. Use a fragrance-free, hypoallergenic moisturiser to maintain the skin's integrity. -
Gentle Cleansing
Avoid harsh scrubs, loofahs, or acidic toners that strip natural protective oils. These can lead to inflammation and micro-abrasions, turning your skin into a breeding ground for pathogens.
Practice Good Hygiene
-
Keep Skin Dry
In Singapore's high humidity, moisture trapped in skin folds (like the armpits, groin, or between toes) provides the perfect environment for fungi (like ringworm) and bacteria to thrive. Use a clean, dry towel to gently pat these areas dry after showering or exercising. -
Post-Gym Hygiene
If you frequent gyms or public pools, shower immediately after your workout. Wear flip-flops in shared locker rooms or communal shower areas to prevent contact with fungal pathogens that cause athlete's foot.
Preventing the Spread of Contagion
-
Do Not Share Personal Items
Fungal and viral infections are easily spread through shared towels, razors, or personal skincare tools. Always use your own items to avoid cross-contamination. -
Hands Off
If you develop a pimple, boil, or suspicious bump, never pick, squeeze, or pop it. This forces bacteria deeper into the tissue (leading to cellulitis) and risks spreading the infection to other parts of your body or to other people. -
Manage Shared Surfaces
If you have an active infection, wash your bedsheets, towels, and clothing in hot water (at least 60°C) to kill lingering fungi or bacteria.
Managing Underlying Health Conditions
-
Optimise Immune Health
If you have systemic health issues like diabetes or poor circulation, strict management of these conditions is critical. High blood sugar levels, for instance, can compromise your immune response and make it significantly easier for skin infections to take hold. -
Protect Minor Wounds
Even small cuts, scratches, or insect bites should be treated immediately. Clean the area with mild soap and water, apply an antiseptic, and keep it covered with a bandage until the skin has fully healed.



When Should You See a Dermatologist for Skin Infections?
While many minor skin issues can be managed with simple hygiene, infections can progress rapidly—especially in Singapore's humid, tropical climate. Certain infections carry a high risk of spreading to deeper tissues or causing systemic illness, making early professional intervention crucial. Please book a consultation if you experience any of the following:
Signs of Spreading Infection
If a red, painful, or warm patch (such as cellulitis) is visibly expanding in size, or if the redness is moving further up your limb.
Presence of Systemic Symptoms
If your skin condition is accompanied by fever, chills, body aches, or swollen lymph nodes, this indicates that the infection is no longer confined to the skin and requires immediate medical attention.
Persistent or Recurrent Infections
If you are dealing with a boil that keeps coming back in the same spot, or a fungal rash (like athlete's foot or ringworm) that does not improve after one week of using over-the-counter anti-fungal creams.
Severe Pain or Throbbing
If a lesion (such as an abscess) becomes so painful that it prevents you from sleeping, walking, or engaging in your normal daily activities.
Infections Near Critical Areas
Any rash, blister, or infection near the eyes, nose, or mouth, or on sensitive areas like the groin or armpits, should be assessed promptly to prevent complications and discomfort.
Uncertain Diagnosis
If you are unsure whether a lesion is a fungal infection, a bacterial boil, or an allergic reaction, do not apply leftover creams or natural remedies. Using a steroid cream on a bacterial or fungal infection will often make it grow significantly faster and more aggressively. A professional exam ensures you get the right medicine for the right invader.
High-Risk Medical History
If you have underlying health conditions such as diabetes, poor circulation, or a weakened immune system, your body's ability to fight off skin infections is reduced. You should see a dermatologist at the earliest sign of any skin breakdown or infection.
FAQs About Skin Infections
Recurring infections are often a sign that your skin's protective barrier or immune response is compromised. Factors like high humidity (common in Singapore), chronic skin conditions (like eczema), or systemic health issues (such as diabetes or poor circulation) can weaken your defences. Additionally, if you frequently engage in activities that involve shared equipment or skin-to-skin contact, your risk of exposure to pathogens is naturally higher.
Yes, most skin infections are contagious. Because they are caused by external pathogens—such as bacteria, fungi, or viruses—they can spread through direct skin-to-skin contact, or indirectly via contaminated surfaces like gym equipment, towels, or communal shower floors. If you suspect an infection, it is best to avoid sharing personal items until a dermatologist has confirmed it is no longer transmissible.
Yes. While some very minor scrapes may heal on their own, delaying treatment is dangerous with skin infections. Bacterial infections like cellulitis can escalate rapidly, and fungal infections rarely clear without targeted intervention. Proper medical treatment is necessary to eradicate the pathogen, prevent scarring, and stop the infection from spreading to other parts of your body or to other people.
Yes. Unlike benign skin growths, which are tied to your personal genetics, skin infections are external invaders. Once the correct pathogen is identified and treated with the appropriate medication (antibiotics, antivirals, or antifungals), the infection is typically cleared. However, you can be re-infected if you are exposed to the same pathogen again or if your skin barrier remains compromised.
Yes. This often happens if the initial treatment was incomplete or if you remain exposed to the source of the infection. For example, if you have athlete's foot and continue to wear the same unsanitised shoes, the fungus will likely return. Following your dermatologist's aftercare instructions and maintaining good hygiene in shared spaces is the best way to prevent the invader from returning.
Seek Proper Dermatologist Care for Skin Infections
If you or your child are experiencing skin infections, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in treatment for skin infections, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh