Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
A wart (verruca) is a common viral skin infection caused by the human papillomavirus (HPV). The virus enters through small breaks in the skin and triggers an overgrowth of skin cells, resulting in thickened, rough lesions. Warts can occur anywhere on the body and may spread through direct contact or from one area of the skin to another.
While some small warts may resolve over time as the immune system clears the virus, others can persist, spread, or become painful—especially when located on weight-bearing areas such as the soles of the feet. With professional dermatological assessment, warts can be accurately identified and treated using targeted methods such as cryotherapy, topical therapies, or procedural treatments.



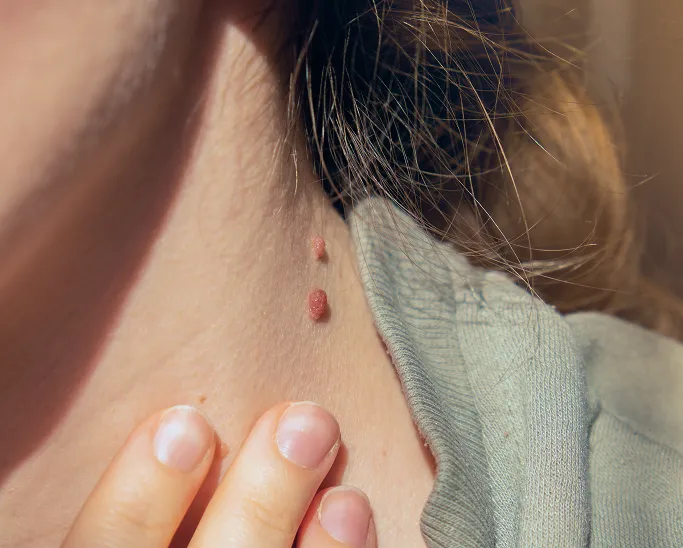
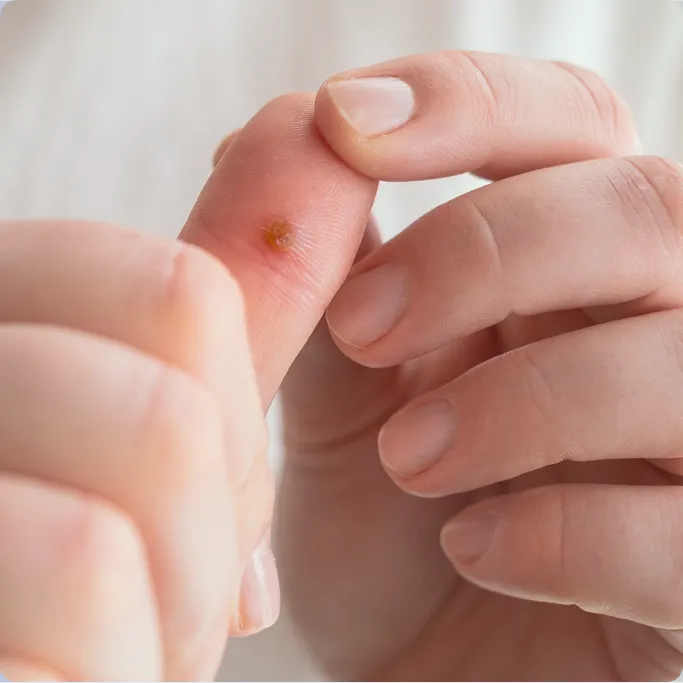
What Is a Viral Wart?
A viral wart is a benign skin lesion caused by HPV that alters the normal growth pattern of skin cells. Clinically, warts often appear as rough, thickened bumps that may be skin-coloured or slightly darker than the surrounding skin.
On the palms and soles, they may contain small black dots, which represent tiny clotted blood vessels. These lesions can become tender or painful due to pressure, particularly in areas subject to friction or weight-bearing.
Because other skin conditions, such as corns or calluses, can resemble warts, an accurate diagnosis is important. A dermatologist can distinguish these based on their clinical features and advise on appropriate management if the lesion is persistent, spreading, or symptomatic.
What Are Common Types of Warts?
Warts are classified by their appearance and the area of the body they affect.
Common Warts (Verruca Vulgaris)
Plantar Warts (Verruca Plantaris)
Plane Warts (Verruca Plana)
Genital Warts (Condyloma Acuminatum)
Mosaic Warts
Common Symptoms of Warts to Look Out For
While viral warts are benign, they can be persistent, physically uncomfortable, and highly contagious. Recognising the signs early can help you seek treatment before the virus spreads to other parts of your body or to other people. Here are the common symptoms to monitor:
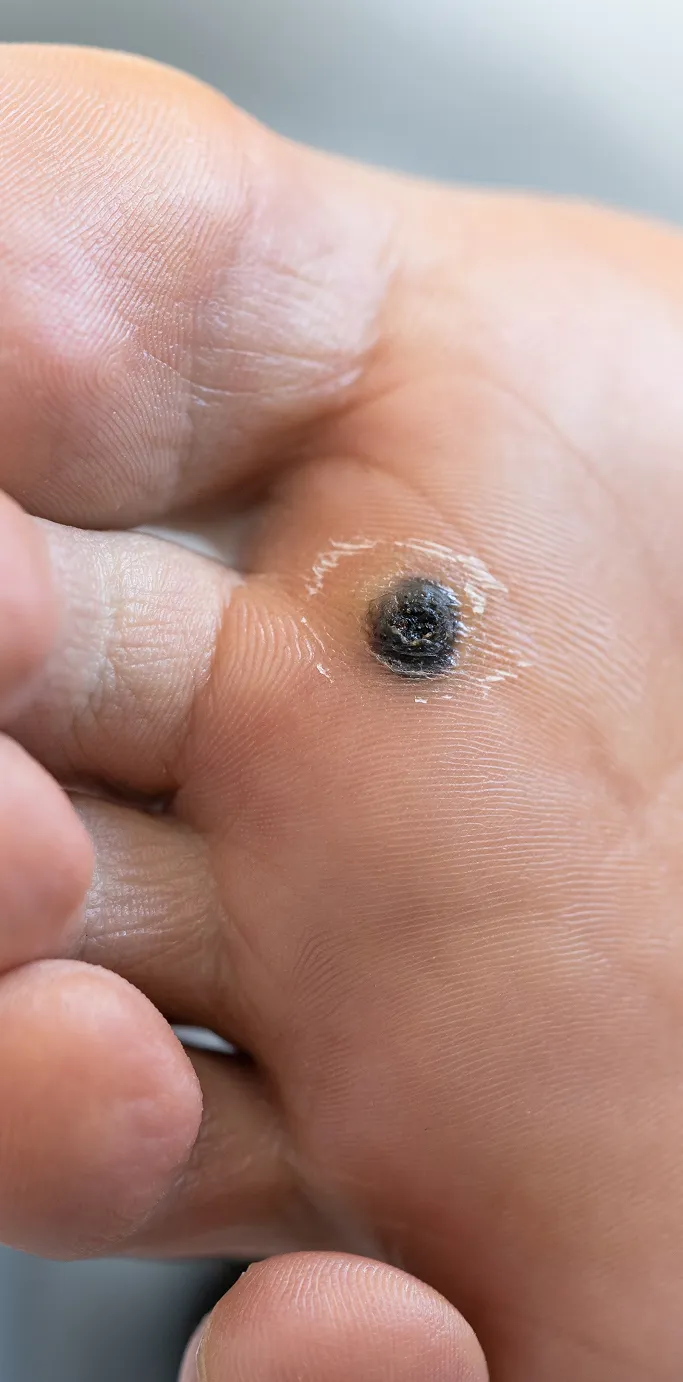
Changes in Skin Texture and Surface
Warts are characterised by an abnormal thickening of the skin. Keep an eye out for:
-
Rough, Grainy Bumps
Look for firm, raised lesions with a cauliflower-like texture. -
Tiny Black Dots
If you notice small, dark specks within a rough growth, these are clotted blood vessels. This is a very common feature of common warts and helps differentiate them from other skin conditions.
Pain and Sensitivity
Most warts are asymptomatic, but they can become painful depending on their location:
-
Pressure-Related Pain
Plantar warts on the soles of the feet often grow inward due to body weight, which can feel like walking on a sharp pebble or a needle. -
Tender Growth
If a wart is located near a fingernail or toenail (periungual), it may become tender or cause the nail to grow in an irregular or brittle manner.
Clustering and Multiplication
Warts are caused by a virus and are prone to spreading:
-
Satellite Lesions
If you notice small, new bumps appearing around a larger, primary wart, this is a sign of autoinoculation—the virus is spreading to the surrounding skin. -
Clusters
Certain types of warts, such as flat warts or mosaic warts, tend to appear in large groups. If you suddenly notice dozens of small, flat bumps on your face, neck, or hands, this warrants a professional assessment.
Disruption of Skin Lines
Persistence and Resistance
Bleeding Upon Trauma
What Causes or Triggers Warts?
While many skin infections are opportunistic, viral warts are specifically driven by HPV. Unlike bacterial or fungal infections that thrive on general surface moisture or skin breaks, HPV is a highly specialised virus that manipulates your skin's own growth cycle.
Autoinoculation (Self-Spread)
One of the most common ways warts multiply is through autoinoculation—spreading the virus from one part of your body to another.
-
Picking and Scratching
When you pick or attempt to peel a wart, the viral load on your fingertips increases. You then inadvertently deposit that virus onto other healthy areas of skin, leading to new wart growth. -
Shaving
Shaving over a cluster of flat warts on the face or legs can create a trail of new warts along the path of the razor.
Indirect Transmission
Warts are notoriously contagious and are frequently spread via fomites (contaminated objects or surfaces). In Singapore's active lifestyle environment, common transmission hubs include:
-
Public Facilities
Wet floors in public swimming pools, gyms, or communal shower areas. -
Shared Equipment
Yoga mats, exercise equipment, or towels that have been used by someone with an active wart. -
Personal Items
Shared razors, nail clippers, or pumice stones can easily transfer the virus from a wart to healthy skin.
HPV Infection and Cellular Hijacking
HPV enters the top layer of the skin (the epidermis). Once inside, the virus hijacks the machinery of your skin cells, forcing them to multiply at an unnaturally rapid rate. This overproduction of cells is what creates the thickened, rough, or cauliflower-like surface of the wart.
Routes of Entry: The Role of Micro-trauma
The virus requires a gateway to enter your skin. This usually occurs through:
-
Micro-abrasions
Tiny, invisible cracks, scratches, or nicks in the skin (often from shaving, scratching, or dry, cracked skin) serve as the perfect entry point for the virus. -
Macerated Skin
Skin that has been softened by prolonged moisture—such as the soles of feet after a long workout or in communal showers—is much more porous and susceptible to viral invasion.
Individual Susceptibility and Immune Status
Not everyone exposed to HPV develops a wart. Your susceptibility depends on:
-
Immune Response
Your body's ability to recognise and fight off HPV varies. If your immune system is temporarily suppressed—due to stress, illness, or certain medications—you are more likely to develop warts. -
Skin Health
Individuals with pre-existing skin conditions, such as atopic dermatitis (eczema), often have a compromised barrier, making it significantly easier for the virus to establish itself.
How Are Warts Diagnosed?
A dermatologist diagnoses viral warts by evaluating their clinical appearance and pattern of distribution. Because warts can sometimes be confused with other skin growths like calluses, corns, or even rare skin cancers, a precise clinical assessment is essential to confirm the presence of the Human Papillomavirus (HPV).
Clinical Examination and Inspection
The primary diagnostic tool is a thorough visual assessment. We look for specific morphological markers:
-
The Black Dot Sign
Using a dermatoscope (a high-powered magnifying device), we look for tiny, clotted blood vessels within the lesion. These appear as small black dots, which are a hallmark sign of a wart, as they represent the capillary supply feeding the rapidly growing viral tissue. -
Disruption of Skin Markings
Warts typically interrupt the normal skin lines (dermatoglyphics). If the natural ridges of your skin seem to disappear or bend around a growth rather than pass through it, it is a strong indicator of a wart.
Diagnostic Differentiation
A critical part of our assessment is distinguishing warts from mimics:
-
Calluses vs. Warts
While both cause skin thickening, calluses are typically uniform, lack clotted blood vessels, and maintain normal skin lines. Warts are often tender when pinched from the sides (rather than pressed directly downward) and show the characteristic black dots under magnification. -
Punch Biopsy
In rare or complex cases—particularly if a growth on the skin does not respond to standard wart treatments, has an irregular border, or displays atypical features—we may perform a punch biopsy. A small tissue sample is taken under local anaesthesia to examine the skin architecture under a microscope, ensuring we rule out other conditions.
Medical History Review
The doctor will ask targeted questions to confirm the diagnosis and identify how the virus may have been contracted:
-
Duration and Evolution
How long has the growth been present? Has it increased in size or have new bumps appeared around it? -
Anatomical Context
Are you noticing them on weight-bearing areas (like the soles of the feet), which might suggest Plantar Warts, or in clusters, which might suggest Flat Warts? -
Lifestyle Factors
Do you frequently use public swimming pools, gym showers, or shared locker rooms? Have you or your household members had similar growths recently?
How Are Warts Treated and Removed at TSN Dermatology?
As warts are caused by the Human Papillomavirus (HPV), our treatment goal is to either destroy the virus-infected tissue or stimulate your immune system to recognise and eliminate the virus itself. Since warts can be persistent and prone to recurrence, we often utilise a combination approach tailored to the type, location, and size of your warts.
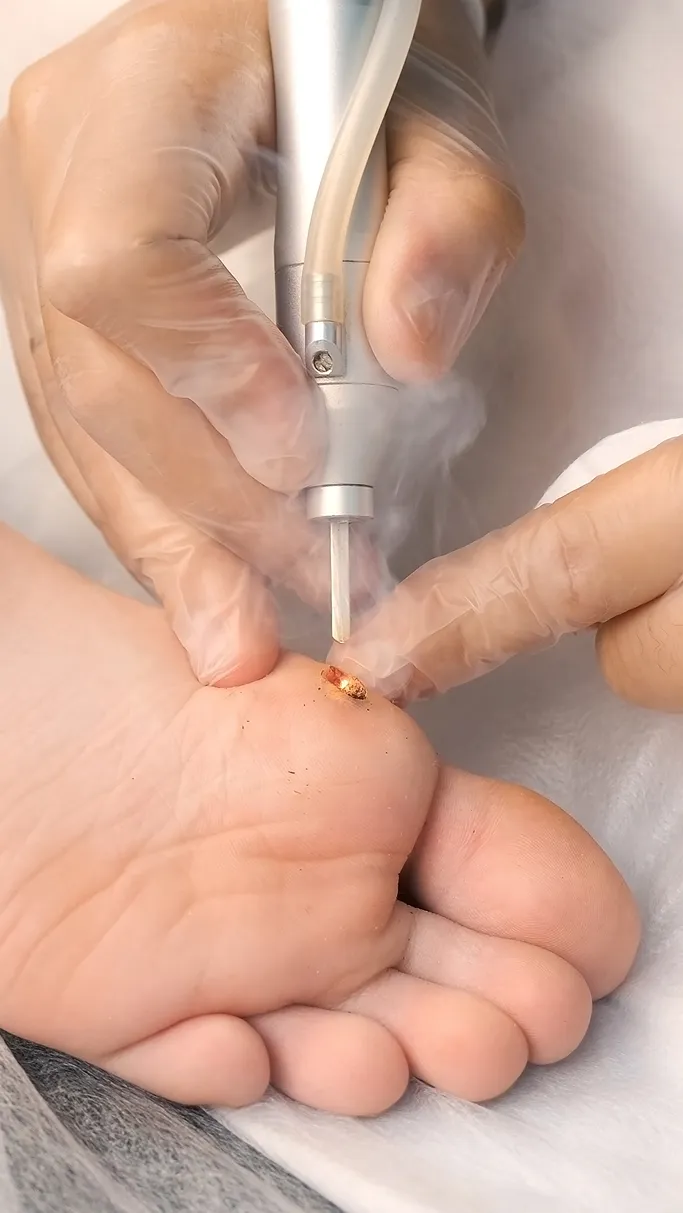
Individualised Treatment Approach
We assess the wart's location—such as the high-pressure soles of your feet versus the sensitive skin of your face—to select the safest, most effective method. Our goal is to achieve clearance while protecting the surrounding healthy skin and minimising the risk of scarring.
Procedural Interventions
For most patients, in-office procedures are the most efficient way to remove visible warts:
Cryotherapy
We use liquid nitrogen to precisely freeze the wart. This induces a controlled inflammatory response that destroys the viral tissue, causing the wart to blister and gradually resolve over time.
Electrocautery
Using a specialised tool, we deliver controlled heat to destroy the wart tissue. This is particularly effective for stubborn, thicker warts and helps seal blood vessels, while minimising bleeding and protecting the surrounding healthy skin.
Laser Therapy
For resistant or widespread warts, medical-grade lasers can target the blood supply feeding the wart, targeting the blood vessels supplying the wart and helping to destroy the affected tissue.
Minor Surgical Removal
For large, isolated, or painful warts that do not respond to other methods, we may perform a minor excision under local anaesthesia to remove the visible lesion.
Topical and Immunotherapy
For certain cases, we utilise medications to treat the viral infection on the surface:
Prescription Topical Treatments: We provide customised lotions or creams (such as high-strength acids or cell-cycle inhibitors) that you apply at home to gradually dissolve the wart.
Immunotherapy: For persistent or recurrent warts, we may use specialised treatments to stimulate your immune system at the site of the lesion. By waking up your immune response, your body learns to attack and clear the HPV virus on its own.
Post-Procedural Care
Proper aftercare is essential to ensure the skin heals smoothly and to prevent the virus from re-establishing itself:
Wound Protection: Following cryotherapy or laser treatment, we provide instructions on keeping the area clean and covered. This is crucial for preventing secondary bacterial infection while the site heals.
Monitoring for Recurrence: Warts can occasionally return if microscopic viral particles remain. We advise a brief follow-up to ensure complete clearance.
Scar Prevention: If a wart is deep (common with plantar warts), we may recommend soothing or regenerative creams to ensure the underlying tissue heals without forming a hard, uncomfortable callus.
Long-Term Prevention
To ensure you remain free of warts, we guide you on how to manage your skin environment:
Hygiene Education: Advice on how to avoid the fomite transmission associated with gyms, pools, and shared equipment.
Skin Barrier Maintenance: Maintaining well-hydrated, intact skin is the best defence against viral entry. We recommend specific non-comedogenic moisturisers to prevent the tiny cracks that HPV exploits.
Avoiding Autoinoculation: We teach you how to properly care for a healing wart site to ensure you do not inadvertently transfer the virus to your fingers or other body parts.
Tips on Daily Care and Prevention of Warts
Since warts are caused by a virus (HPV) that exploits breaks in your skin and spreads through direct or indirect contact, prevention is largely about barrier protection and hygiene. In Singapore's tropical climate, where we are often barefoot or in shared fitness environments, these habits are essential to keeping your skin virus-free.
Protect Your Natural Barrier
-
Keep Skin Moisturised
A well-hydrated skin barrier is far more resilient. Dry, cracked skin—especially around the heels and fingers—provides easy entry ports for the HPV virus. Use a gentle, fragrance-free moisturiser daily to keep your skin supple and intact. -
Avoid Micro-Trauma
Shaving over warts or dry, callused skin creates tiny nicks that allow the virus to enter or spread. If you must shave, use a sharp, clean razor and avoid passing over any suspicious bumps.
Practice Good Hygiene
-
Wear Protective Footwear
Never walk barefoot in public locker rooms, swimming pools, or communal showers. These are prime environments for HPV transmission. Wear rubber flip-flops to create a physical barrier between your skin and contaminated surfaces. -
Post-Activity Care
If you use public gym equipment or yoga mats, wipe them down before and after use. Thoroughly wash your hands and feet after exercising in shared facilities to remove any potential viral contaminants.
Preventing Self-Spread
-
Hands Off
If you have a wart, never pick, chew, or cut at it. This is the most common reason warts multiply. Picking breaks the skin and forces the virus into the surrounding tissue or onto your own fingertips, leading to a cluster of new warts. -
Careful Grooming
If you have a wart, do not use the same nail clippers, pumice stones, or emery boards on that area and then on healthy skin. If you must use a tool on a wart, dedicate it exclusively to that area and disinfect it thoroughly, or use disposable files.
Managing Exposure Risks
-
Do Not Share Personal Items
HPV can survive on towels, razors, and skincare tools. To prevent cross-contamination, never share personal hygiene items, even with close family members. -
Keep Warts Covered
If you have an active wart, keep it covered with a bandage or plaster, especially in environments where you might have skin-to-skin contact with others (like sports or fitness classes). This significantly reduces the risk of the virus jumping to someone else.
Early Intervention
-
Don't Wait and See
Viral warts are much easier to treat when they are small and few in number. If you notice a suspicious rough patch that is not going away, schedule a professional assessment. Avoiding DIY bathroom surgery is key to preventing the deeper infection and scarring that often results from improper removal attempts.



When Should You See a Dermatologist for Warts?
While many warts are benign, they can be persistent, unsightly, and prone to spreading. Because they are caused by a virus (HPV) and thrive in humid climates like Singapore, it is often difficult to eradicate them completely without professional guidance. Please book a consultation if you experience any of the following:
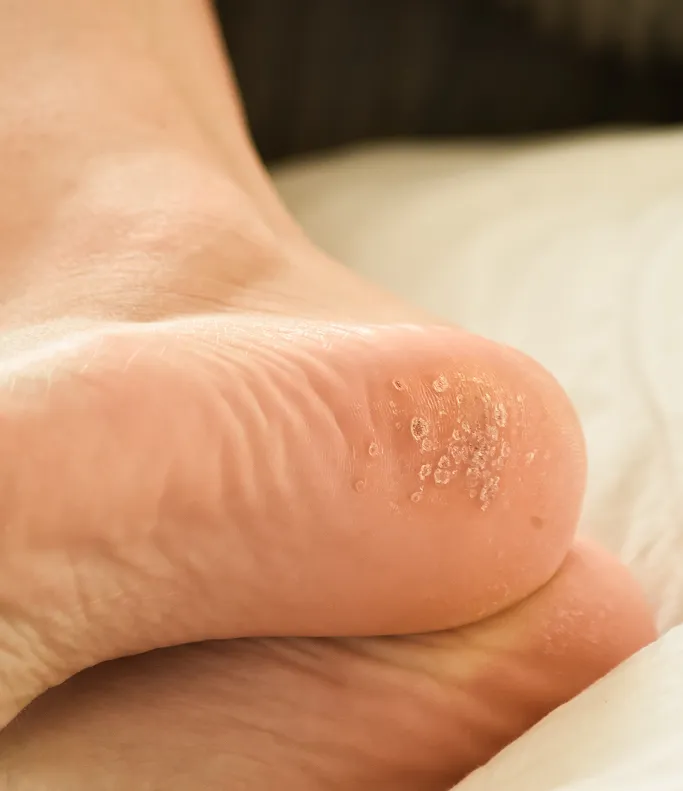
Warts That Are Spreading
If you notice new warts appearing near an existing one (autoinoculation) or if they are spreading to other parts of your body, professional treatment is necessary to break the cycle of infection.
Pain or Discomfort
If a wart on your foot (Plantar Wart) makes walking painful, or if a wart near a fingernail (Periungual Wart) causes tenderness or affects nail growth, you should seek professional removal to restore comfort and function.
Warts That Fail to Respond to Home Treatment
If you have used over-the-counter wart paints, plasters, or freezing kits for several weeks without success, the virus is likely too deep or resilient for surface-level treatment. Continued home treatment often leads to skin irritation without clearing the virus.
Atypical or Changing Growths
If a growth changes colour (e.g., turns dark or variegated), bleeds frequently, or has an irregular border, it requires an urgent examination to rule out skin cancers that can occasionally mimic the appearance of a wart.
Warts on Sensitive or Cosmetic Areas
Warts on the face, neck, or in the genital region require specialised care. Attempting to treat these areas at home can lead to permanent scarring, pigment changes, or the inadvertent spread of the virus to sensitive mucosal tissue.
High-Risk Medical History
If you have diabetes, poor circulation, or a compromised immune system, you should never attempt to treat warts (especially on the feet) at home. Your body is less efficient at healing, and any injury—no matter how small—can lead to secondary bacterial infections or slow-healing wounds.
Uncertain Diagnosis
If you are unsure if a bump is a wart, a corn, a mole, or something else, please avoid the wait-and-see approach. A professional dermatological exam provides an accurate diagnosis, ensuring you don't accidentally treat a benign mole or a malignant lesion with harsh wart-removing acids.
FAQs About Wart Removal
Yes. Warts are caused by the Human Papillomavirus (HPV). Because they are viral, they can spread through direct skin contact or contaminated surfaces. They can spread through direct skin-to-skin contact with an infected person or indirectly through contaminated surfaces (fomites) like shared gym equipment, yoga mats, or wet floors in public showers and swimming pools.
Warts can be successfully cleared with treatment, but because they are caused by a virus, curing them is different from treating a bacterial infection. Our goal is to remove the visible lesion and stimulate your immune system to recognise and fight the HPV virus. While the treated wart will not return, it is possible to develop new warts in the future if you are re-exposed to the virus or if dormant viral particles in the surrounding skin become active.
While some very small warts might eventually resolve on their own as your immune system matures, we generally recommend professional treatment. This is because warts are prone to spreading to other parts of your own body (autoinoculation) or to other people. Professional intervention ensures the lesion is removed safely without damaging the healthy skin around it, which helps reduce the risk of spreading the virus.
You can try OTC treatments for very mild, isolated warts, but we advise caution. OTC products often contain strong acids that do not distinguish between viral tissue and healthy skin. If applied incorrectly, they can cause significant chemical burns, scarring, or pigment changes. If you have been using an OTC product for a few weeks without improvement, or if you have a wart on your face, neck, or genital area, please stop and see a dermatologist to avoid permanent skin damage.
Yes. Recurrence is common if the virus was not fully eradicated or if the skin in that area remains susceptible to viral entry. For example, if you have a plantar wart and continue to walk barefoot in high-risk areas, the virus can easily re-infect the same site. Maintaining healthy, intact skin and following your dermatologist's aftercare plan is the best way to prevent the virus from re-establishing itself.
Seek Proper Dermatologist Care for Wart Removal
If you are concerned about a wart or a new skin growth, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can evaluate the area, confirm the diagnosis, and discuss suitable treatment options. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in warts removal, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh