Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
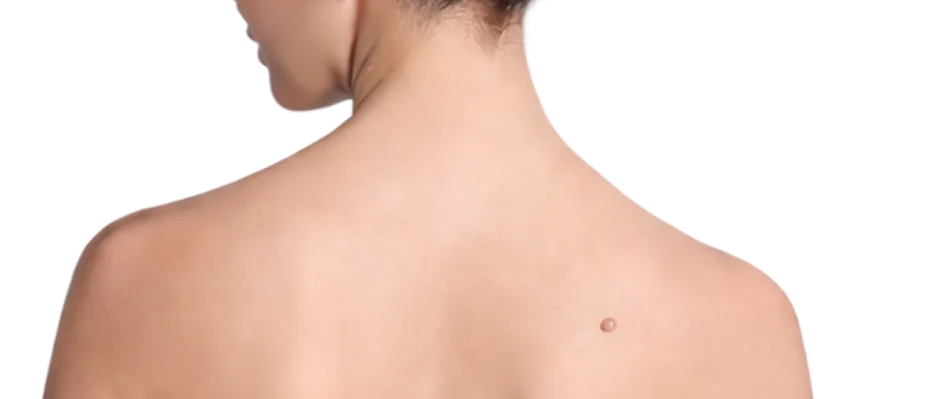
A cyst is a common dermatological concern that often presents as a persistent, slow-growing lump within the cutaneous layers. While these growths are typically asymptomatic and non-malignant, they represent a structural change in the skin's anatomy rather than a temporary blemish. Proper clinical identification is essential, as the presence of an internal sac distinguishes a true cyst from other common skin conditions, such as lipomas or localised infections, necessitating a specific medical approach for effective resolution.



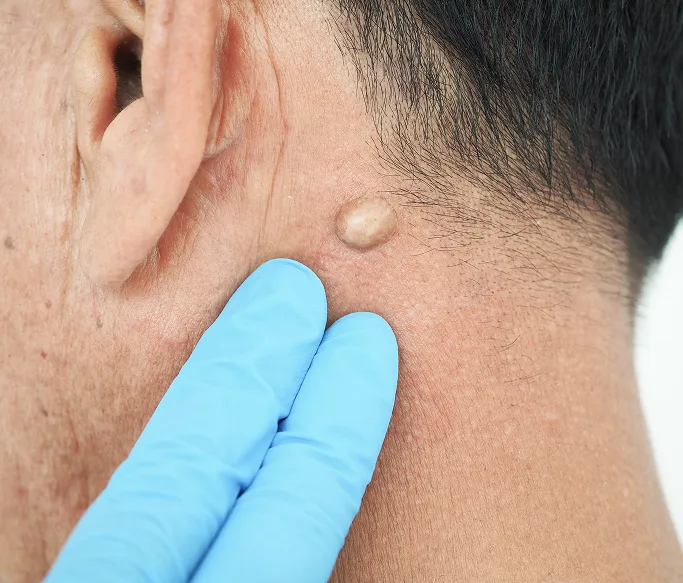
What Are Cysts?
Cysts are common, generally benign (non-cancerous) skin growths that present as closed, sac-like pockets of tissue. While they can occur anywhere on the body, they are most frequently found on the face, neck, back, and trunk. Visually, cysts usually appear as round, dome-shaped lumps that lie beneath the skin's surface. Depending on their contents, they can feel firm or fluctuant (moveable) to the touch.
In many cases, a cyst may have a visible central pore on the overlying skin. If a cyst is squeezed—though this is strongly discouraged—a whitish, malodorous material may discharge from this opening. While many people mistake them for persistent acne, cysts possess a surrounding capsule or lining that requires specialised dermatological intervention to remove permanently. Without professional excision of this capsule, the cyst is highly likely to recur.
What Are Common Types of Cysts?
Cysts are not a single, uniform condition. They are clinically classified based on their anatomical origin, the type of lining (capsule) they possess, and the material they contain. Identifying the specific type is essential for determining the most effective method for permanent surgical removal.
Epidermal (Sebaceous) Cysts
This is the most common subtype, and they are often referred to as sebaceous cysts, though they are technically filled with keratin rather than sebum. They appear as firm, dome-shaped lumps beneath the skin and frequently feature a central pore. They can occur anywhere on the body where hair follicles are present, particularly the face, neck, and trunk.
Trichilemmal (Pilar) Cysts
These cysts are structurally similar to epidermal cysts but arise from the middle layer of the hair follicle. They are almost exclusively found on the scalp. Because the skin on the scalp is thicker, pilar cysts often feel very firm or stone-like and are more likely to be multiple. They are often hereditary and tend to have a thicker capsule, making them easier to remove intact.
Acne Cysts (Pseudocysts)
While frequently called cysts, these are clinically classified as pseudocysts because they lack a true epithelial lining. They occur during severe inflammatory acne flare-ups when an oil gland or follicle ruptures deep within the dermis. Unlike true cysts, these are highly inflammatory and prone to causing significant scarring if not treated with specialised dermatological injections or systemic therapy.
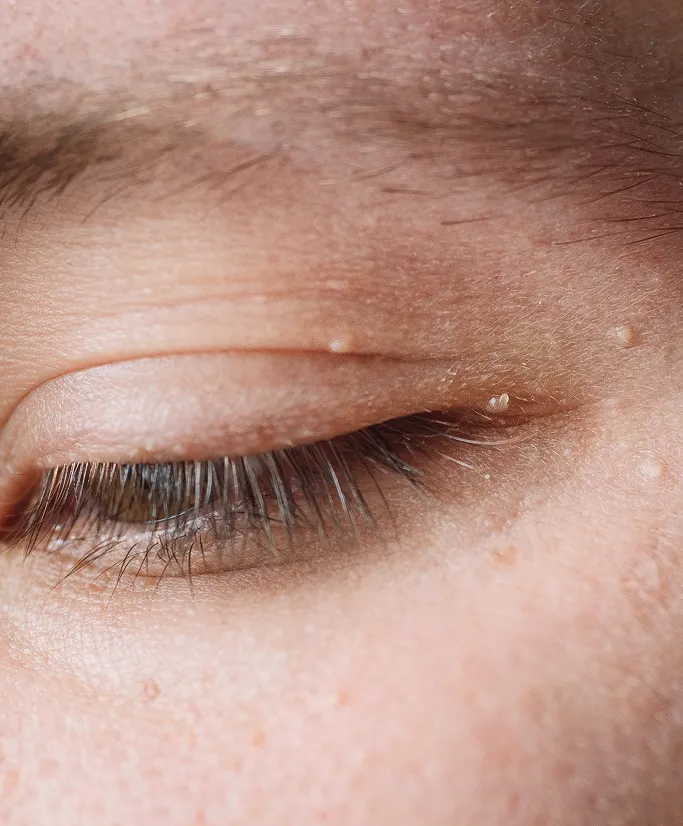
Milia (Tiny Epidermal Cysts)
Milia are essentially miniature epidermal cysts. They appear as small, firm, pearly white bumps, typically around the eyes and cheeks. They occur when keratin becomes trapped just below the surface of the skin. While they are harmless, they are often a cosmetic concern and require professional extraction, as they do not pop like standard acne.
Digital Mucous Cysts
These are specialised cysts that occur near the joints of the fingers or at the base of the fingernail. They are filled with a clear, jelly-like fluid (mucin). Because of their proximity to the nail matrix, they can sometimes cause a groove or deformity in the growing nail. These require careful surgical management to avoid affecting the joint or nail growth.
Dermoid Cysts
A more complex type of cyst that is present from birth, although it may not be noticed until later in life. These cysts can contain various types of tissue, including hair, skin glands, or even tooth-like structures, as they form during embryonic development. They are most commonly found on the face, particularly near the eyebrow or the midline of the neck.
Common Symptoms of Cysts to Look Out For
Cysts are typically slow-growing and asymptomatic, but they present specific clinical features that distinguish them from other dermatological conditions. Monitoring these signs is essential for determining when a cyst requires professional intervention to prevent complications.
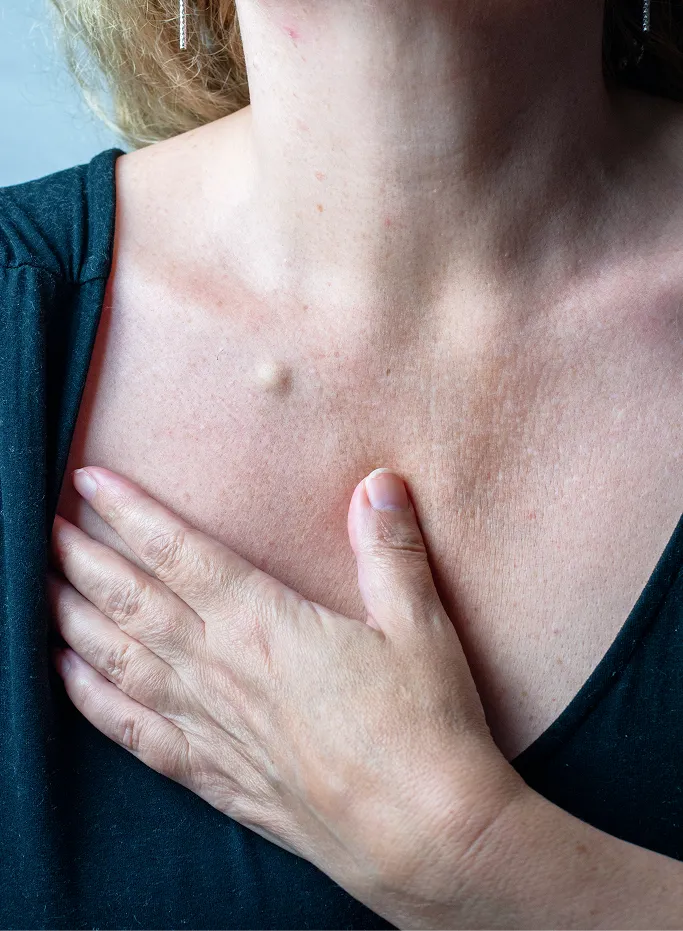
Discrete Subcutaneous Lump
The most characteristic sign is a round, dome-shaped lump located just beneath the skin's surface. These growths are usually mobile, meaning you can slightly move the lump under the skin with your fingers. While often firm, some cysts may feel fluctuant or fluid-filled depending on the thickness of the internal keratin.
Central Punctum (Pore)
Many epidermal cysts feature a small, darkened opening at the apex of the lump, known as a punctum. This represents the blocked duct of the hair follicle from which the cyst originated. In some cases, this pore may remain visible even if the cyst is not currently inflamed.
Malodorous Discharge
If a cyst is compressed or ruptured, it may extrude a thick, cheesy, or yellowish material. This substance is primarily composed of keratin (skin protein) and often has a distinct, unpleasant odour. This discharge is a clear indicator that the growth is a cyst rather than a solid tumour or lipoma.
Acute Inflammation and Redness
While a quiet cyst is skin-coloured and painless, it can become acutely inflamed if the internal wall ruptures. Symptoms include sudden redness, warmth, and significant tenderness around the lump. This stage often mimics a localised infection or a boil and requires immediate dermatological care to manage the inflammation.
Pain and Tenderness
A stable cyst is generally painless. However, pain can arise if the cyst grows large enough to press on surrounding nerves, or if it is located in a high-friction area (such as the beltline or underarms). Sudden, sharp pain is usually a sign of internal rupture or secondary bacterial infection (abscess formation).
Recurring Flares
Patients often notice that a cyst appears to drain and flatten out, only to refill and return several weeks or months later. This occurs because the internal lining (the capsule) remains intact. As long as the sac is present, it will continue to produce keratin and cause the cyst to reform.
Scalp Bumps (Pilar Cysts)
If you notice firm, smooth, and often multiple lumps on the scalp, these are likely pilar cysts. Because the scalp skin is taut, these cysts can become quite hard and may be felt more easily when brushing or washing your hair. Unlike facial cysts, they rarely have a visible central pore.
What Causes or Triggers Cysts?
The development of a cyst is fundamentally a structural event rather than a temporary infection. It occurs when skin cells, rather than shedding naturally, move deeper into the skin and multiply, creating a sealed pocket or sac. This sac then begins to produce and trap keratin—the protein that normally forms the skin's surface—leading to the formation of a localised lump.
Follicular Blockage: The Primary Mechanism
Localised Skin Trauma
Genetic Predisposition
Hormonal Influence and Acne History
Inflammation and Friction
Developmental Factors
What Usually Happens to a Cyst?
Cysts are generally unpredictable in their behaviour; while some remain stable for years, others may undergo cycles of inflammation or gradual enlargement. Understanding the natural progression of a cyst is essential for deciding when to move from observation to surgical intervention.
Stabilisation and Growth Patterns
The Risks of Squeezing and Manual Expression
It is a common misconception that a cyst can be popped like a standard pimple. Patients should strictly avoid squeezing a cyst. Attempting to manually drain it often forces the keratin and bacteria deeper into the surrounding dermis rather than out through the pore. This leads to:
-
Cyst Rupture
Breaking the internal capsule wall. -
Severe Inflammation
A foreign body reaction as the immune system attacks the released keratin. -
Acute Pain and Swelling
Transforming a quiet lump into a painful, red abscess. -
Recurrence
Since the lining (the capsule) is not removed, the cyst will inevitably form back again, often with more scar tissue, which makes future surgical removal more complex.
Anatomical Vulnerability and Rupture
Cysts located in high-pressure or high-friction areas are at a significantly higher risk of spontaneous rupture.
-
Back and Shoulders
Pressure from sitting against chairs, lying down, or wearing backpacks can cause the cyst wall to fail. -
Thighs and Beltline
Constant friction from clothing and movement makes these cysts prone to inflammation. -
Scalp
Frequent brushing or grooming can irritate pilar cysts.
Due to this high risk of painful rupture and subsequent infection, dermatologists typically recommend the elective removal of cysts in these high-traffic areas before they become symptomatic.
Spontaneous Inflammation (The Flare)
How Are Cysts Treated at TSN Dermatology?
The primary goal of cyst management is to provide a permanent solution while achieving the best possible cosmetic outcome. While many cysts are benign and can be safely left alone, professional dermatological assessment is essential to determine if intervention is needed.
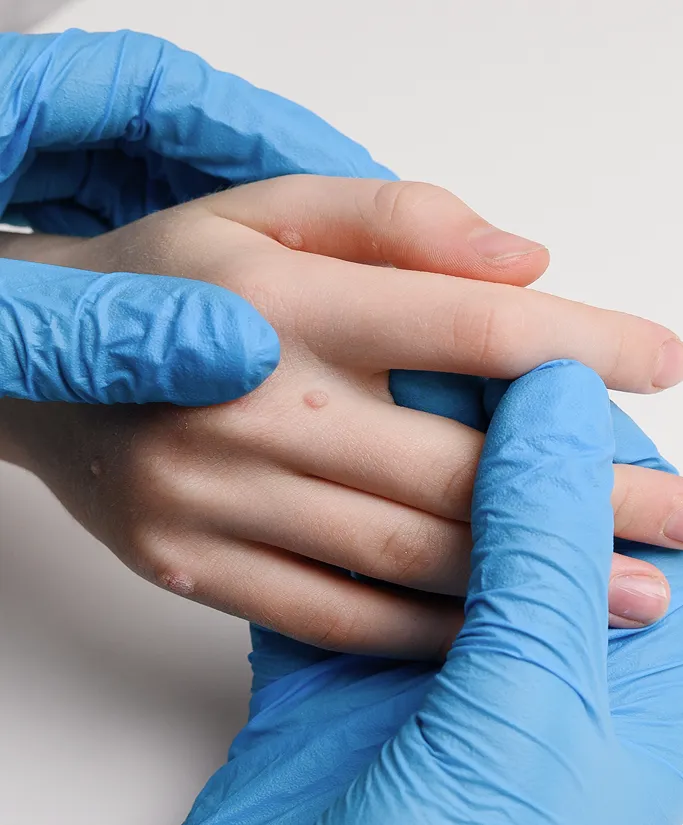
The Importance of Complete Excision
It is important to understand that simple incision and drainage—often performed in emergency settings for acute abscesses—is usually inadequate for long-term resolution. Because the underlying sac (the capsule) remains, the cyst is highly likely to recur. At TSN Dermatology, our focus is on complete surgical excision, which involves removing the entire sac lining to ensure the cyst does not return.
The Day-Surgery Process
Cyst removal is a straightforward, low-risk procedure performed in our clinic under local anaesthesia as a day-surgery. The process is designed to be efficient and comfortable:
- Surgical Technique: A small incision is made directly over the cyst. The skin is gently stretched apart to locate the cyst sac, which is then dissected and removed in its entirety, including its complete lining.
- Minimal-Scar Approaches: For average-sized, non-inflamed cysts, our surgeons utilise a mini-incision technique. By creating a smaller opening, we can extract the cyst and close the site with only a few fine stitches. This significantly reduces the size of the final scar compared to traditional methods.
Management of Inflamed or Infected Cysts
If a cyst has already ruptured or become infected, the tissue can be too fragile for immediate excision. In these cases, we may first manage the inflammation with:
Intralesional Steroid Injections
To rapidly reduce swelling and pain.Incision and Drainage (I&D)
To provide immediate pressure relief for an abscess.Follow-up Excision
Once the acute inflammation has fully subsided, we will plan a definitive complete surgical excision to ensure the cyst does not reform.
Specialised Care for Specific Types
Milia Extraction
These tiny, surface-level cysts are managed through gentle extraction with a sterile micro-needle.Pilar (Scalp) Cysts
Because these have a thicker wall, they are often excellent candidates for a quick pop-out excision through a small scalp incision.Acne Pseudocysts
Managed primarily through medical therapy and targeted injections, as they lack the true anatomical sac found in epidermal cysts.
Tips on Daily Care and Prevention of Cysts
While most cysts are benign, they can be persistent and prone to painful complications if ignored. Because cysts are structural growths, they cannot be cured with skincare or diet; however, adopting the right habits can prevent irritation, reduce the risk of infection, and manage asymptomatic cysts until professional removal can be scheduled.
The Hands-Off Rule
-
Do Not Squeeze or Pop
This is the most critical rule. Squeezing a cyst almost never removes the internal lining and often forces the contents deeper into the skin. This triggers a severe inflammatory response, increases the risk of infection, and creates more scar tissue, which makes subsequent professional removal significantly more difficult. -
Avoid Constant Palpation
Frequently touching, rubbing, or pressing on the cyst to see if it has changed can irritate the skin barrier and inadvertently cause the internal wall to rupture.
Preventing Irritation and Friction
-
Clothing Choices
If you have a cyst on your back, chest, or shoulders, avoid tight-fitting synthetic clothing that creates friction or traps heat. Opt for loose, breathable fabrics to prevent the cyst wall from becoming inflamed. -
Watch for Pressure Points
Be mindful of how your daily habits affect the cyst. For instance, if you have a cyst on your back, avoid sitting in chairs that put direct pressure on the lump. If it is on your thigh, try to shift your seating position to avoid friction. -
Gentle Grooming
If you have a pilar cyst on the scalp, be gentle when brushing or washing your hair. A hard blow from a hairbrush can easily rupture an exposed cyst.
Lifestyle and Prevention
-
Maintain Healthy Skin
While you cannot prevent a cyst from forming, keeping your skin healthy through regular cleansing and exfoliation (where appropriate) helps prevent the clogging of hair follicles that often precedes cyst development. -
Sun Protection
Always keep your skin protected with SPF. While UV does not cause cysts, protecting your skin ensures that if you do require a minor surgical excision, your skin is in the best possible condition for rapid, scar-minimised healing.
Monitoring for Changes
-
Observe Growth Patterns
Keep an eye on any rapid changes. While cysts are typically slow-growing, a sudden increase in size or a rapid change in shape warrants a professional check-up. -
Track Inflammation
Note if the cyst becomes red, warm, or suddenly tender. These are the earliest signs that the internal wall may have breached, and early medical intervention (such as an anti-inflammatory injection) can often prevent a full-blown abscess. -
Keep the Area Clean
Maintain good hygiene around the cyst. A simple, gentle cleanser used during your shower is sufficient. Avoid applying harsh acne treatments, astringents, or alcohol-based toners to the cyst, as these will only irritate the skin surface without affecting the sac underneath.
When to Seek Early Intervention
-
High-Traffic Locations
If your cyst is in an area prone to trauma (like the beltline or under the arm), consider having it removed electively while it is quiet and uninflamed. It is always faster and easier to remove an uninfected cyst than to manage a painful, infected one. -
Signs of Infection
If you notice spreading redness, pus-like discharge, or if you develop a fever, contact our clinic immediately. These symptoms indicate the cyst has become an abscess and requires urgent medical drainage and possibly antibiotics.



When Should You See a Dermatologist for Cysts?
While most cysts are harmless and can be monitored, they have the potential to become painful, infected, or aesthetically bothersome. It is important to know when a cyst requires professional assessment to ensure you receive the safest and most effective care.
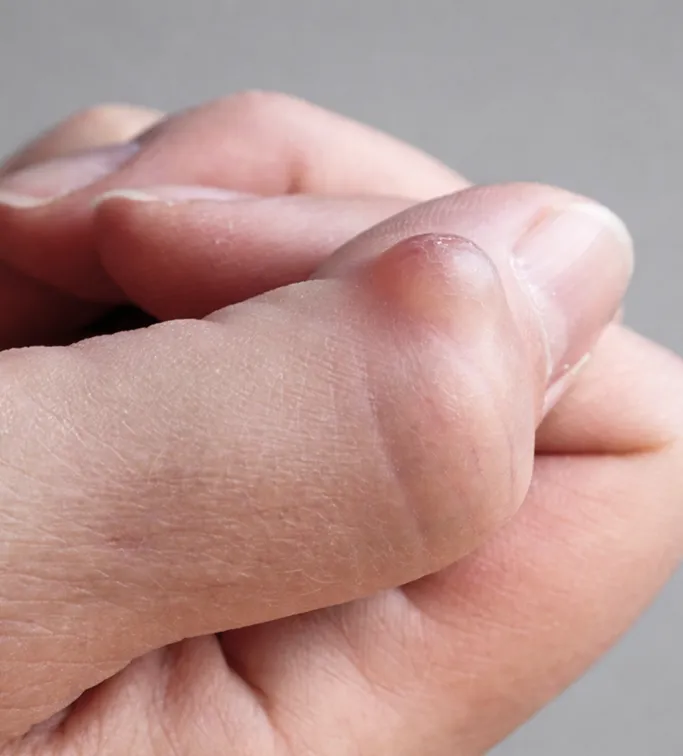
Signs of Acute Inflammation
Seek medical care if you notice sudden redness, warmth, increasing pain, or swelling around your cyst. These symptoms often indicate that the internal sac has ruptured and is at high risk of developing into a painful abscess.
Persistent Pain or Tenderness
If the cyst is consistently causing you discomfort or pain, it may be pressing on nearby nerves or be located in a high-friction area that is prone to irritation.
Rapid Changes in Size
While most cysts grow slowly, any sudden or rapid increase in size should be evaluated. Rapid expansion can sometimes indicate a more complex underlying issue that requires a diagnostic biopsy.
Recurrent Rupture and Discharge
If your cyst has leaked or drained on its own multiple times, it is a sign that the capsule is compromised and will continue to cause issues. Ongoing self-drainage increases the risk of chronic infection and thick, irregular scarring.
Inconvenient or High-Friction Locations
If your cyst is located on your back, legs, underarms, or along the beltline, it is constantly being subjected to pressure and friction. We recommend early evaluation for these cysts to remove them electively before they have the chance to rupture.
Aesthetic Concern
If the lump is in a highly visible area, such as your face, neck, or ears, and it is causing you self-consciousness or distress, we can discuss minimally invasive removal techniques that prioritise a discreet, clean cosmetic result.
Uncertain Diagnosis
If you are unsure whether a lump is a cyst, a lipoma (fatty growth), or another type of lesion, a professional dermatological assessment is necessary to confirm the diagnosis. Treating a lump blindly—especially by squeezing it—can lead to unnecessary complications.
Signs of Infection (Systemic)
If you develop a fever, chills, or see spreading red streaks extending from the cyst site, seek immediate medical attention. This is a sign that an infection may be spreading into the surrounding skin, requiring urgent treatment.
FAQs About Cysts
No. Skin cysts are not infections and cannot be spread through physical contact or sharing personal items. They are benign, self-contained structural abnormalities within your own skin layers, typically arising from a localised blockage or developmental variation.
No. Squeezing a cyst is strongly discouraged. Because a cyst is enclosed in a sac (the capsule), squeezing it will not remove the lining. Instead, it often forces the contents deeper into the surrounding tissue, which triggers intense inflammation, increases the risk of a painful infection, and creates more scar tissue. A cyst that has been squeezed almost always recurs.
A cyst will continue to recur as long as the sac wall (the capsule) remains intact beneath the skin. Even if you manage to drain the fluid or cheese-like material, the sac continues to produce keratin. Permanent removal requires surgical excision of the entire sac, which our surgeons perform as a standard day-surgery procedure.
Most true epidermal or pilar cysts do not disappear on their own. While they may occasionally drain if they become inflamed, they are anatomical structures that will likely persist or refill over time. If a cyst is in a high-friction area or causes aesthetic concern, elective surgical removal is the most reliable way to resolve it.
For a permanent solution, yes. Surgical excision—where the entire cyst sac is removed—is the only way to guarantee the cyst will not return. While intralesional steroid injections can help shrink a cyst that is acutely inflamed or painful, they do not remove the sac itself and are typically used as a bridge to calm the area before definitive surgical removal.
Yes. Any full-thickness skin surgery will leave a small scar. However, by using mini-incision techniques and precise surgical closure, our fellowship-trained surgeons can keep these scars as discreet as possible. The resulting scar is almost always preferable to the risk of a large, irregular, and potentially infected scar caused by a spontaneous cyst rupture.
Seek Proper Dermatologist Care for Cysts
If you or your child are experiencing Cysts, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in cyst removal surgery, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh