Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
What Is Mohs Micrographic Surgery?
Mohs micrographic surgery is an advanced, tissue-sparing technique used to treat cutaneous malignancies with a high degree of precision. Originally developed by Dr Frederic E. Mohs in the 1930s and refined over decades of clinical practice, this technique is internationally recognised as the gold standard for the surgical management of high-risk skin cancers.
Unlike traditional wide local excision, which relies on pre-determined margins, Mohs micrographic surgery offers a superior oncological outcome by providing real-time, comprehensive microscopic control of the surgical margins. This approach achieves the highest cure rates for skin cancer while simultaneously prioritising the preservation of healthy, non-cancerous tissue.
Mohs surgery is specifically indicated for complex, high-risk, or recurrent skin cancers. It is particularly essential for lesions located on the face, scalp, ears, nose, and lips, where achieving clearance while minimising the excision size—and therefore the final scar—is critical.
Tissue Preservation
Microscopic Verification
Optimal Reconstruction



How Does Mohs Micrographic Surgery Work?
Mohs micrographic surgery operates on the principle of complete margin control, treating the removal of skin cancer as a precise, three-dimensional mapping process rather than a standard excision. In many high-risk or recurrent skin cancers, malignant cells—often referred to as subclinical extensions—can grow in unpredictable, finger-like projections deep into the dermis, far beyond what is visible to the naked eye. Traditional surgery relies on a safety margin that estimates the tumour's boundary, which can inadvertently result in the removal of too much healthy tissue or, conversely, leaving behind microscopic pockets of disease.
Mohs micrographic surgery is mostly performed by fellowship-trained dermatological surgeons. In Mohs surgery, cancer tissue is removed layer by layer and examined under the microscope on the same day. Further tissue is only removed if remaining cancer cells are seen. This means healthy, cancer-free tissue is not sacrificed. After the doctor is satisfied that no more cancer cells are seen, the wound can be closed. The dermatologic surgeon is also trained to perform reconstruction of the wound, using various methods such as skin flaps or grafts.
Mohs surgery intercepts this uncertainty through an integrated, same-day cycle of excision and microscopic analysis:
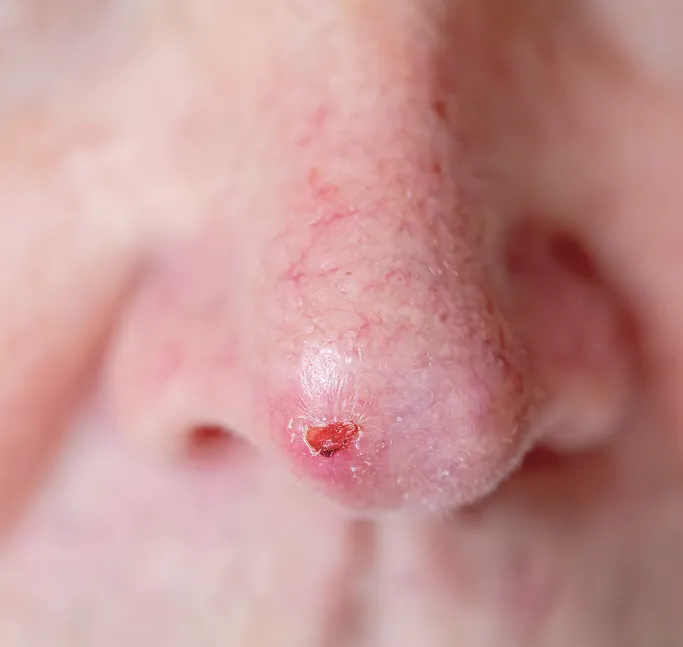
Layered Excision
The surgeon removes the visible tumour along with a very narrow margin of tissue. This tissue is meticulously mapped and colour-coded to correspond to the exact orientation on the patient's body.
Microscopic Verification
The tissue is processed in our on-site laboratory. The Mohs surgeon, acting as both the oncologist and the pathologist, examines 100% of the tissue margins under the microscope. This allows us to see exactly where cancer cells exist and where the tissue is healthy.
Targeted Removal
If the microscopic analysis reveals any remaining malignant cells, the surgeon identifies their exact location and removes only those specific areas. This surgical precision preserves the maximum amount of healthy surrounding tissue, which is vital for both functional and aesthetic outcomes in delicate areas like the nose, eyelids, ears, and lips.
Beyond merely removing the tumour, the Mohs technique provides a comprehensive reset for the skin. Once the surgeon confirms the margins are microscopically clear, the body's healing environment is no longer compromised by malignant growth. The reconstruction phase then allows the surgeon to utilise advanced techniques—such as local tissue flaps or grafts—to restore the site's structural integrity and aesthetic contour, resulting in the smallest possible scar and the highest potential for long-term cure.
How Is Mohs Micrographic Surgery Performed at TSN Dermatology?
The Mohs micrographic surgery process at TSN Dermatology is a highly disciplined, systematic procedure designed to provide the highest oncological cure rate while optimising functional and aesthetic restoration. Performed as a same-day surgery under local anaesthesia, the procedure is uniquely precise, allowing us to map the tumour's true extent in real-time. Fasting is not required, and our team will have previously reviewed your medications to advise which may be continued on the day of surgery.
The Procedural Stages
- Preparation and Initial Excision
The surgical site is numbed with a local anaesthetic, ensuring the procedure is painless. Once prepared, the surgeon marks the visible skin cancer and removes it along with a very narrow margin of healthy-appearing skin. This constitutes the first Mohs stage. - On-Site Laboratory Analysis
The excised tissue is meticulously colour-coded and mapped to maintain its exact orientation relative to your body. It is immediately sent to our adjoining laboratory, where it is sectioned, stained, and mounted onto microscope slides. This laboratory processing can take up to 2 hours, depending on the size and thickness of the tissue. - Patient Comfort During Processing
While the laboratory processes the tissue, your wound will be dressed, and you may leave the operating room to relax in our dedicated waiting area with your family members and enjoy refreshments.
- Microscopic Verification and Targeted Excision
The surgeon personally examines the slides to trace 100% of the surgical margins. If microscopic tumour cells remain, the surgeon identifies their exact location on the map. You will be brought back to the operating room for a targeted, minimal excision of only the remaining malignant tissue. This cycle of excision and testing repeats until the margins are confirmed to be completely clear of malignancy. The majority of cases are completed within three stages. - Reconstructive Closure
Once we confirm the cancer is fully eradicated, we move to the final stage: reconstruction. Your surgeon, who is fellowship-trained in both oncology and reconstructive techniques, will restore the integrity of the wound using the most appropriate method—whether it be primary linear closure, natural healing (for small wounds), local tissue flaps, or skin grafts—to ensure the best functional and cosmetic outcome.
Which Skin Cancers Are Suitable for Mohs Micrographic Surgery?
Mohs micrographic surgery is the gold standard for treating skin cancer, specifically when the preservation of healthy tissue and the achievement of the highest possible cure rate are the primary goals. While standard surgical excision is effective for many lesions, Mohs surgery is specifically indicated for high-risk, complex, or cosmetically sensitive cases where tumour borders are challenging to delineate or where recurrence rates must be minimised.
Our fellowship-trained surgeons recommend Mohs micrographic surgery for the following presentations:
Anatomical Location
Large or Deep Lesions
Ill-Defined Borders
Aggressive Histological Features
Recurrent Skin Cancers
Patients with Compromised Immunity
Skin cancer on the face, in particular, requires a unique surgical strategy. Because the tissue is limited and the structural integrity of features like the nose or ears is fragile, taking an extra margin to be safe is often not a feasible option. Mohs surgery eliminates the guesswork; instead of taking a wide safety margin, we take the smallest possible amount of tissue and verify the clearance microscopically. This ensures the best possible outcome for both the complete removal of the cancer and the subsequent reconstructive success.
Patient Preparation & Aftercare for Mohs Micrographic Surgery
To ensure the most successful oncological outcome and the best possible cosmetic healing, we have established clear guidelines for your surgical journey. Proper preparation and diligent post-operative care are essential to ensure the wound heals effectively and remains free of infection.
Pre-Surgical Preparation
Your preparation in the days leading up to your surgery directly impacts the efficiency of the procedure and the quality of your recovery.
-
Medication Management
Please provide a complete list of your current medications and supplements. Specifically, if you are taking blood thinners (e.g., aspirin, clopidogrel, warfarin, or certain herbal supplements like fish oil or Vitamin E), please inform us, as these may need to be temporarily adjusted to minimise bleeding during surgery. -
Smoking Cessation
If you are a smoker, we strongly advise you to stop at least 2 weeks before and after surgery. Smoking constricts blood vessels and drastically reduces oxygen delivery to the skin, which is the leading cause of poor wound healing and increased risk of infection. -
Logistics & Comfort
Mohs surgery is a day-surgery procedure, but because the processing of tissue slides takes time, you should plan to be at the clinic for the majority of the day. Wear comfortable, loose-fitting clothing and arrange for someone to transport you home, as you may be wearing a bulky pressure dressing afterwards. -
Fast and Hydrate
You may eat a light meal and drink water on the day of your surgery. Being well-hydrated and having eaten will help you feel more comfortable during the intermittent waiting periods while our lab processes your tissue samples.
Post-Surgical Aftercare
Supporting the Healing Process Once your surgery and reconstruction are complete, your body begins the complex work of tissue repair. Your post-operative care is the final, vital step in ensuring a successful outcome.
-
The No-Strain Rule
For the first 1-2 weeks, avoid heavy lifting, vigorous exercise, or activities that require bending over. Tension is the enemy of a healing surgical wound; excessive movement can cause the stitches to pull, the wound to bleed, or the final scar to widen. -
Wound Protection
Keep the surgical site and the pressure dressing clean and dry for the duration specified by your surgeon (usually 24-48 hours). Do not submerge the wound in baths, swimming pools, or the ocean, as this significantly increases the risk of bacterial infection. -
Pain and Swelling Management
It is normal to experience some swelling or bruising around the site, particularly if the surgery was on the face. You may use a cold compress gently near the site (but not directly on it) to reduce discomfort. Use only the pain relief medication approved by your surgeon. -
Suture Care & Follow-Up
Follow your specific wound care regimen—typically involving the application of a prescribed healing ointment—and return for your scheduled suture removal appointment. This is also when we perform a final clinical check of the site to ensure optimal healing. -
Long-Term Protection
Once the skin has healed, the scar will remain photosensitive for several months. In Singapore's tropical climate, you must use a broad-spectrum SPF 50+ sunscreen and wear a hat or seek shade. UV radiation is the primary cause of scar hyperpigmentation; protecting the area is crucial to ensuring your scar fades to the best possible cosmetic finish.
What Are The Side Effects of Mohs Micrographic Surgery?
Mohs micrographic surgery is widely considered the gold standard for the treatment of skin cancer due to its exceptional cure rates and precise tissue preservation. While it is a highly controlled surgical procedure, all skin surgeries carry a specific risk profile. Mohs surgery is generally considered a low-risk procedure. Because the amount of healthy tissue removed is significantly less than in traditional wide excision surgery, the risks—such as the extent of the wound and post-operative inflammation—are comparatively lower. Like all skin surgeries, there is a small risk of bleeding, localised infection, and post-operative discomfort after the anaesthesia wears off. If you experience discomfort, our doctors will prescribe appropriate pain relief to ensure you remain comfortable during your recovery.
Common Post-Operative Effects
Swelling and Bruising: Most common for surgeries on the face or near the eyes, this is a normal part of the body's inflammatory healing response. It may appear significant in the first 48 hours but typically resolves on its own within a week.
Sensation Changes: You may experience temporary numbness, tingling, or pins and needles around the surgical site. This occurs because superficial sensory nerves can be disrupted during excision. On the face, particularly, small nerves run beneath the skin; depending on the tumour's location and depth, these may be affected. Your surgeon will advise you if this risk is specifically relevant to your case, and in most instances, feeling gradually returns as the nerves regenerate over several months.
Suture Marks: Depending on skin tension and location, you may see small, track-like marks from the sutures. These generally fade significantly as the scar matures and remodels.
Potential Complications
Wound Infection: While we perform surgery in a sterile environment, infection can occur if the wound is exposed to bacteria. Watch for spreading redness, increasing heat, pus-like discharge, or an increase in pain several days post-surgery. Contact our clinic immediately if you notice these signs.
Scarring: Any full-thickness excision will leave a scar. While our surgeons utilise plastic surgery closure techniques to minimise their appearance, individual healing patterns vary, and some patients may develop raised (hypertrophic or keloid) scars based on their genetic predisposition.
Bleeding (Hematoma): Although rare, a collection of blood can form beneath the skin flap or graft. If the site suddenly becomes firm, tender, or rapidly swollen, notify us immediately.
Rare Risks
Tissue Necrosis: In complex reconstructions, there is a very small risk that transferred tissue may not receive adequate blood supply and could fail. This risk is notably higher in patients who smoke or have conditions that affect circulation.
Scar Stretching: If the wound is in a high-tension area (such as the back, chest, or joints) and the no-strain policy is not followed during the first two weeks, the scar may widen as it matures.
Long-Term Considerations
Skin Cancer Recurrence: While Mohs surgery offers the highest cure rates, no treatment is 100% guaranteed. Because skin cancer is often a marker of extensive cumulative UV damage, there remains a lifelong risk of developing new lesions in surrounding or distant areas. This is why our long-term surveillance and regular professional skin screenings remain a non-negotiable part of your ongoing care.
FAQs About Mohs Micrographic Surgery
Mohs surgery is widely considered a very safe, low-risk procedure. It is performed under local anaesthesia, which avoids the risks associated with general anaesthesia. Because the technique is so precise, the resulting wounds are often smaller, leading to fewer complications and faster healing times compared to traditional wide excisions.
No. While both involve surgically removing the tumour, the key difference lies in the margin control. In a standard excision, the tissue is removed and sent to an outside lab, with results taking several days. In Mohs surgery, 100% of the surgical margins are examined microscopically by the surgeon on the same day. This real-time analysis ensures the cancer is completely removed while preserving the maximum amount of healthy tissue.
The procedure itself is painless because the area is thoroughly numbed with local anaesthesia. You will remain awake and alert throughout the day. Once the anaesthesia wears off, most patients experience only mild discomfort or a tightness at the site, which is typically well-managed with standard over-the-counter pain relief.
The main concern involves medications that affect blood clotting. Certain antibiotics, anti-inflammatories, and blood thinners (like aspirin or warfarin), as well as some herbal supplements, can increase the risk of bleeding during and after surgery. It is critical to provide our team with an updated list of all your medications so we can provide specific instructions on what to continue or pause.
Consult a Dermatologist for Skin Cancer Management
If you require evaluation or treatment for skin cancer, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic will help establish an accurate diagnosis and determine whether Mohs micrographic surgery is the most appropriate approach. Please contact us for more information or to arrange an appointment.

Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh

